What Happens If the Amygdala Is Damaged? Symptoms, Causes, and Brain Function Effects

Medically reviewed by Laura Athey Updated Date: March 27, 2026
In my years of clinical practice, I have often discussed the amygdala as the brain’s “smoke detector.” It is an ancient, almond-shaped structure deep within the temporal lobe that scans our environment for danger.
Most of my patients come to me because their smoke detector is too sensitive—triggering the “fight-or-flight” response at the slightest hint of stress. However, there is a fascinating and medically significant flip side to this: what happens if the amygdala is damaged?
When the amygdala is compromised, the brain’s primary alarm system goes silent. Imagine standing on the edge of a precipice or facing a growling predator and feeling absolutely nothing—no racing heart, no sweaty palms, and no urge to retreat.
While this might sound like a superpower to someone struggling with an anxiety disorder, it is actually a profound neurological deficit that fundamentally alters how a person interacts with the world, makes decisions, and connects with others.
Understanding the symptoms and causes of amygdala damage isn’t just about mapping brain injury; it’s about understanding the very fabric of human emotion and survival.
What Does the Amygdala Normally Do?
Before we explore the consequences of injury, we must understand the baseline amygdala function. In a healthy brain, the amygdala serves as the gatekeeper of the limbic system. Its responsibilities are multifaceted:
- Emotional Processing: It assigns “feeling” to our experiences. It is particularly adept at processing high-arousal emotions like fear and aggression.
- Threat Detection: It operates on a “low road” of neural processing, meaning it can detect a threat and trigger a physical response in milliseconds—well before the rational executive function of the prefrontal cortex can catch up.
- Memory Formation: It works in tandem with the hippocampus to “tag” memories with emotional significance. This is why you vividly remember your wedding day or a car accident, but likely forgot what you ate for lunch three weeks ago.
- Social Intelligence: It helps us interpret subtle social cues, such as the “look” of fear or untrustworthiness on a stranger’s face.
What Happens If the Amygdala Is Damaged?

The question of what happens if the amygdala is damaged depends heavily on whether the damage is unilateral (one side) or bilateral (both sides). If the damage is extensive, a person may develop what is known in neurology as Klüver-Bucy syndrome.
The Core Effects of Damage
- Diminished Fear Response: This is the hallmark symptom. A person with amygdala damage may no longer recognize dangerous situations. They might handle venomous snakes or walk into dark, dangerous alleys without the protective surge of adrenaline that keeps most of us safe.
- Emotional Agnosia: This is a specific type of “emotional blindness.” Patients often struggle to recognize emotions in others, particularly fear. If they see a photo of someone screaming in terror, they might describe the person as “surprised” or “confused.”
- Hyper-orality and Hyper-sexuality: In some cases of bilateral damage, individuals may develop a tendency to examine objects by mouth or show inappropriate sexual behaviors, as the “brakes” on their primal impulses have been removed.
- Impaired Decision-Making: Because our choices are often guided by “gut feelings” (somatic markers), the lack of an emotional compass makes it difficult to weigh risks versus rewards.
Symptoms of Amygdala Damage
In a clinical setting, symptoms of amygdala damage can be subtle at first, appearing more like a personality shift than a typical medical illness. I often observe that while the person’s IQ and logic remain intact, their “social-emotional IQ” plummets.
Common Clinical Presentations:
- Inappropriate Trust: An inability to detect “red flags” in people, leading the person to be easily exploited.
- Blunted Affect: A “flatness” in their own emotional expression; they may seem indifferent to both tragedy and joy.
- Reduced Personal Space Awareness: Patients may stand uncomfortably close to others, as the amygdala usually regulates the “discomfort” we feel when our boundaries are crossed.
- Poor Impulse Control: A tendency to act on immediate desires without the secondary “fear of consequences” that usually prevents risky behavior.
How Amygdala Damage Affects Emotions
This is the main topic of our exploration, and it requires a deep dive into the “why” of our neurobiology. To understand how amygdala damage affects emotions, we have to recognize that the amygdala is the bridge between a physical sensation and a mental “feeling.”
The Blunting of the “Salience” Signal
In a healthy brain, the amygdala acts as a highlighter. When something happens—a loud bang, a kind word, or a beautiful sunset—the amygdala “highlights” that information as important.
When the amygdala is damaged, that highlighter runs dry. Life becomes a series of facts without feeling. This is often described as a blunted fear response, but it is more accurately a loss of emotional salience.
Why Fear Disappears
The biological reason fear vanishes is due to the interruption of the HPA axis (Hypothalamic-Pituitary-Adrenal axis).
Normally, the amygdala sends a distress signal to the hypothalamus, which then triggers the release of cortisol and adrenaline. Without that initial signal, the body never gets the memo that it needs to be in “survival mode.”
The Psychology of Social Recognition
Emotion is our primary social currency. We rely on our amygdala to interpret the micro-expressions of those around us. For a patient with a damaged amygdala, social interactions become exhausting and confusing.
It is like watching a movie in a foreign language without subtitles; they can see the action (the facial movements), but they cannot translate the meaning (the emotion). This leads to a profound sense of social isolation, as the person can no longer participate in the shared emotional language of humanity.
One nuance I frequently share with my patients is the relationship between the amygdala and circadian rhythms. While physical damage is rare, “functional damage” from chronic sleep deprivation is incredibly common.
Sleep is when the prefrontal cortex “re-syncs” with the amygdala. Without adequate rest, the amygdala becomes hyperreactive, mimicking some of the impulsive behaviors seen in damaged cases, but in reverse—over-triggering instead of under-triggering.
I once worked with a patient, “Robert,” whose trauma history had left his amygdala in a state of constant high alert. We found that simply stabilizing his sleep hygiene significantly improved his ability to process emotions, proving that even a “stressed” amygdala has remarkable neuroplasticity.
Real-Life Examples of People With a Damaged Amygdala
Perhaps the most famous example in neuropsychology is the case of Patient S.M., a woman who had a rare condition that caused her amygdalae to calcify and wither away.
In my study of this case and similar clinical observations, the behavior is striking. S.M. was famously described as “the woman who knows no fear.” Researchers took her to haunted houses, showed her horror films, and even exposed her to live snakes and spiders. She reported no fear; in fact, she showed an intense curiosity.
What will happen if the amygdala of a person, like S.M.’s, is such that the very concept of “danger” becomes an abstract idea rather than a felt reality?
S.M. had been held at knifepoint and gunpoint on different occasions but felt no trauma or lingering anxiety afterward. While this sounds like resilience, it actually put her in repeated danger because her brain couldn’t “learn” to avoid high-risk people or places.
Amygdala Damage Compared to Other Brain Structures
To understand the specificity of the amygdala, we must compare it to its neighbors.
| Brain Structure | Function | Effect of Damage |
| Amygdala | Emotional appraisal/Fear | Loss of fear; social/emotional “blindness.” |
| Hippocampus | Conscious memory/Facts | Anterograde amnesia (inability to form new memories). |
| Thalamus | Sensory relay station | What happens if the thalamus is damaged? Total sensory loss, or “thalamic pain syndrome.” |
| Prefrontal Cortex | Logic/Inhibition | Drastic personality changes; loss of impulse control (e.g., Phineas Gage). |
In clinical practice, I often see patients who confuse what happens if the hippocampus is damaged with amygdala issues. If your hippocampus is damaged, you’ll forget the fact that a stove is hot. If your amygdala is damaged, you’ll remember the stove is hot, but you won’t feel the fear or hesitation that stops you from touching it again.
What Causes Amygdala Damage?
While the amygdala is tucked away safely deep in the temporal lobe, it is not invincible. In my practice, I find that understanding the “how” behind the injury helps patients and families navigate the long-term behavioral changes.
The causes of amygdala damage can range from sudden trauma to progressive neurological conditions.
Primary Medical Causes:
- Ischemic Stroke: A blockage of blood flow to the temporal lobe can cause localized cell death within the amygdala.
- Traumatic Brain Injury (TBI): Significant impact or “shearing” forces from accidents can damage the delicate neural pathways connecting the amygdala to the rest of the brain.
- Viral Encephalitis: Specifically, the herpes simplex virus (HSV) has a known affinity for the temporal lobes and can lead to rapid bilateral damage.
- Epilepsy Surgery: In cases of severe, drug-resistant epilepsy, a temporal lobectomy (removing part of the temporal lobe) may inadvertently involve the amygdala.
- Urbach-Wiethe Disease: A rare genetic condition that causes the amygdala to calcify and harden over time, essentially turning the “smoke detector” into stone.
What Causes an Overactive Amygdala?
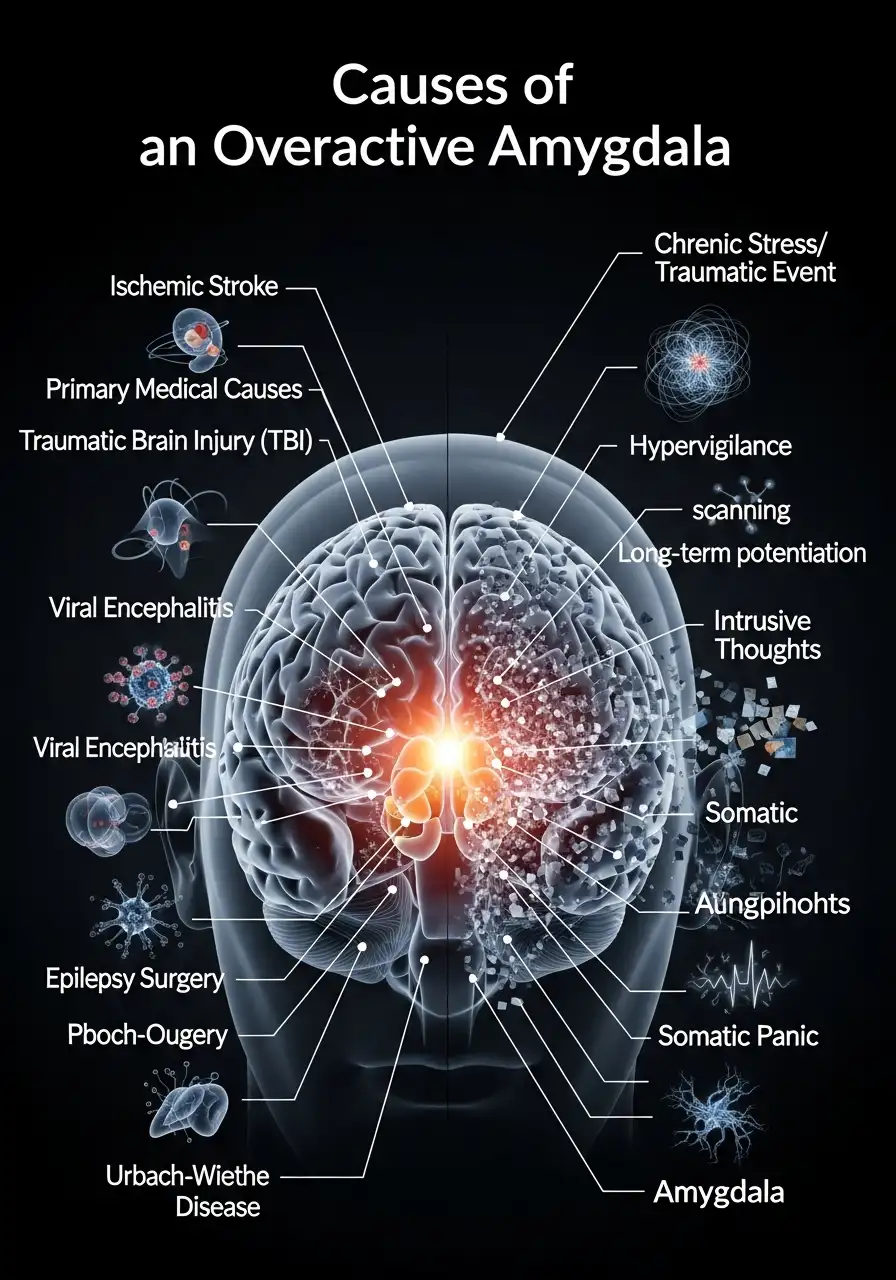
It is equally important to distinguish between physical damage and functional “misfiring.” What causes an overactive amygdala is rarely a physical lesion and more often a response to environmental conditioning.
When a person experiences chronic stress or a singular traumatic event, the amygdala’s neural pathways are strengthened—a phenomenon known as long-term potentiation. The brain essentially “learns” to stay in a state of high alert. This leads to the symptoms of an overactive amygdala, which include:
- Hypervigilance: Constantly scanning for “threats” that aren’t there.
- Intrusive Thoughts: The amygdala forces traumatic memories into the conscious mind.
- Somatic Panic: Sudden bursts of adrenaline, chest tightness, and rapid heart rate.
Can the Amygdala Be Healed or Repaired?
A question I am frequently asked is, “Can the amygdala be healed?” The answer is nuanced and deeply rooted in the concept of neuroplasticity.
If the neurons within the amygdala have been physically destroyed by a stroke or surgery, those specific cells do not regenerate. However, the brain is remarkably adaptable.
Through a process called “functional reorganization,” other parts of the brain—often the prefrontal cortex or the opposite amygdala—can begin to compensate for the lost functions.
How to “Repair” Amygdala Function:
- Cognitive Behavioral Therapy (CBT): This helps “retrain” the brain to evaluate threats logically rather than reactively.
- Pharmacotherapy: Medications like SSRIs can help lower the “baseline noise” of a hyper-reactive amygdala, creating space for healing.
- Neurofeedback: This specialized therapy allows patients to see their brain waves in real-time, teaching them to consciously lower the “electrical volume” of their emotional centers.
Functional Damage: When the Amygdala Misinterprets Reality in Bipolar Disorder
In clinical neuroscience, “damage” doesn’t always refer to a physical lesion or a traumatic brain injury.
In the context of Bipolar Disorder, the amygdala often suffers from functional damage—a state where the structure remains intact, but its “software” or signaling process becomes fundamentally compromised. This leads to a profound misinterpretation of reality, where the brain’s alarm system loses the ability to distinguish between a genuine threat and a neutral event.
During a manic or depressive episode, the communication lines between the amygdala and the prefrontal cortex (the logical “brakes” of the brain) effectively fray. This creates a state of social-emotional blindness. For a person with Bipolar Disorder, the amygdala may “misfire” while reading a loved one’s facial expression.
A neutral look can be misinterpreted as anger or judgment, triggering an immediate, intense defensive response. This isn’t a choice; it is the biological result of a “damaged” signaling pathway that perceives hostility where none exists.
Furthermore, this functional impairment severely impacts risk assessment. In a healthy brain, the amygdala sends a “caution” signal when we consider a dangerous or impulsive action. In Bipolar mania, this signaling is often silenced or bypassed.
The brain loses its natural inhibitory feedback, leading to the high-stakes impulsivity—financial, social, or physical—that characterizes the disorder. The amygdala isn’t physically missing, but for the duration of the episode, its role as a reliable guardian of reality is functionally offline.
Frequently Asked Questions
What happens if the amygdala is damaged?
You may lose the ability to feel fear or recognize it in others. This often leads to increased risk-taking, inappropriate social behavior, and a “blunted” emotional life.
What are the symptoms of amygdala damage?
Common symptoms include an inability to detect danger, difficulty reading facial expressions (especially fear), and an unusual lack of anxiety or “gut feelings” in risky situations.
Can a damaged amygdala be repaired?
While dead neurons cannot be replaced, the brain can use neuroplasticity to form new pathways. Therapy and rehabilitation can help patients “relearn” emotional recognition and social boundaries.
What causes amygdala damage?
The most common causes are stroke, traumatic brain injury, certain viral infections (like encephalitis), and rare genetic conditions.
What happens if the hippocampus is damaged?
Unlike the amygdala (emotion), the hippocampus controls facts. Damage here results in anterograde amnesia, where you can no longer form new memories of people, places, or events.
Conclusion
The amygdala is a vital sentinel, a guardian that has kept our species safe through millennia of evolution. When it is damaged, the silence of the “smoke detector” is not a peace—it is a vulnerability.
However, whether we are dealing with a brain that is too quiet (damage) or a brain that is too loud (anxiety), the human capacity for change is immense.
By understanding what happens if the amygdala is damaged, we gain deeper insight into the fragile, beautiful mechanics of human connection and survival.
Authoritative References
- National Institute of Mental Health (NIMH)
- National Institutes of Health (NIH) – Brain Injury
- American Psychological Association (APA)
- Harvard Medical School – The Emotional Brain
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.










