What Causes Emotional Dysregulation? Symptoms, Types, and How to Treat Them

Imagine being triggered by a minor event—perhaps a partner forgetting to pick up milk or a child spilling juice—and feeling your emotions instantly spiral out of control. It isn’t just a flash of annoyance; it is a physical takeover.
Your heart races, your vision narrows, and you feel a surge of rage or despair that is entirely disproportionate to the situation. For those who are unable to regulate emotions, this isn’t a choice; it is a daily reality that impacts mental health, career stability, and the very fabric of their relationships.
In my practice as a clinical psychologist, I often observe that patients feel a profound sense of shame regarding these “explosions” or “meltdowns.” They describe a labile mood—one that shifts like quicksand—leaving them feeling exhausted and misunderstood. Whether we are discussing an adult overwhelmed at work or a child struggling in the classroom, understanding what causes emotional dysregulation is the first step toward moving from a state of constant “hijack” to a state of agency.
This guide explores the neurobiological roots, the environmental triggers, and the evidence-based strategies that allow for lasting change.
Causes of Emotional Dysregulation
When patients ask, “What causes emotional dysregulation?” I explain that we have to look at the brain as a complex electrical circuit. In a well-regulated brain, the prefrontal cortex (the “logical manager”) maintains a steady connection with the amygdala (the “emotional alarm”). In a dysregulated brain, that connection is frayed or delayed.
Childhood Factors and the Developing Brain
The foundation of emotional control is laid in early childhood through a process called co-regulation. If a child grows up with caregivers who are emotionally immature, inconsistent, or abusive, the child’s nervous system stays in a state of “high alert.”
- Early Stress Exposure: Chronic stress in early life can physically alter the development of the brain, leading to a hyper-reactive amygdala.
- Parenting Styles: If a child’s big emotions are met with punishment or dismissal, they never learn the executive function skills necessary to self-soothe. Instead, they learn to suppress emotions until they eventually “boil over.”
Adult Factors and Neurobiology
In adults, what causes emotional dysregulation is often a combination of that childhood foundation and current biological stressors.
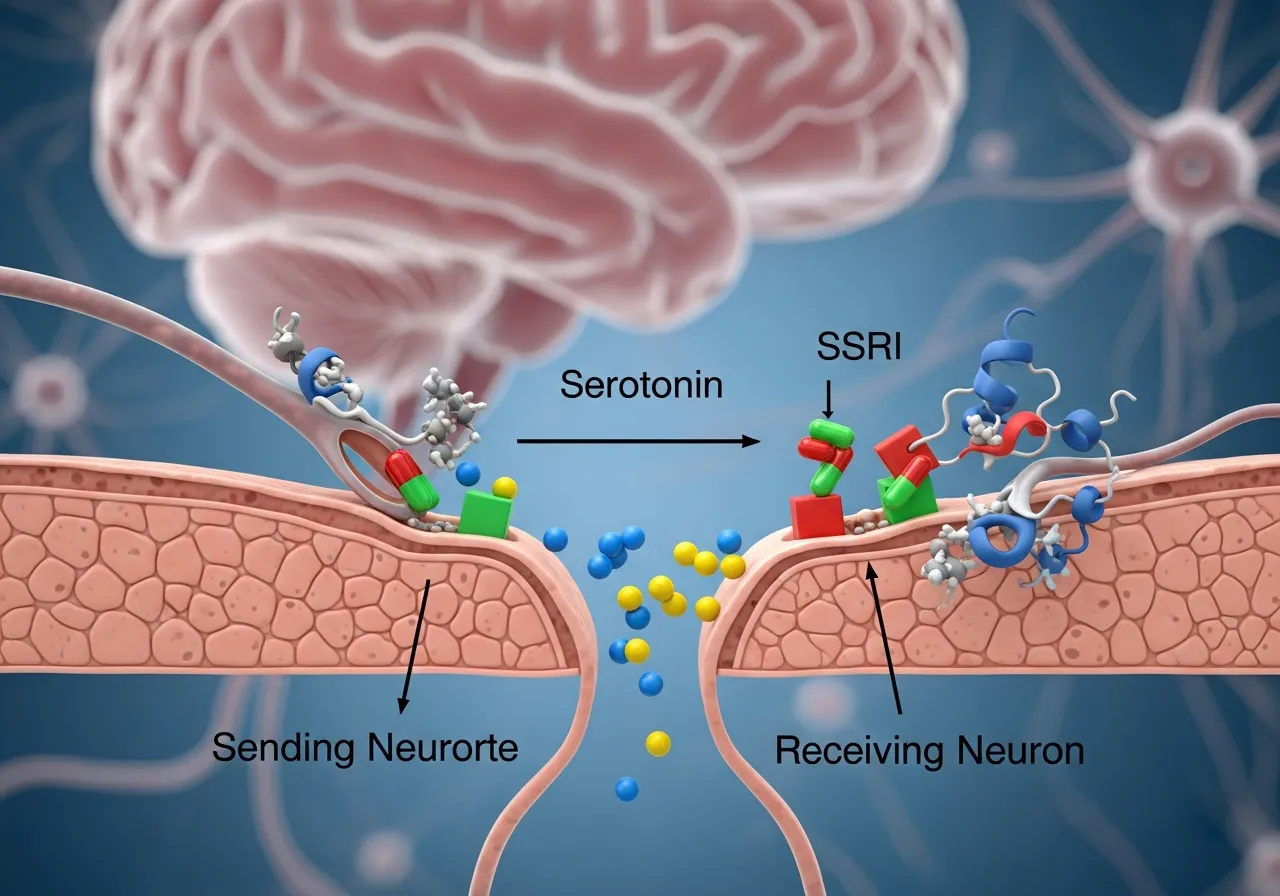
- Neurochemical Imbalances: Fluctuations in dopamine and serotonin—the brain’s “reward” and “mood” chemicals—can make the emotional “floor” feel very unstable.
- Hormonal Shifts: In my practice, I often observe that transitions such as puberty, postpartum, or perimenopause significantly exacerbate dysregulation symptoms.
Condition-Specific Causes: ADHD, Autism, and Trauma
Perhaps the most frequent question I receive is, “What causes emotional dysregulation in ADHD or autism?”
- ADHD: The primary driver here is executive function deficits. The ADHD brain struggles with “inhibition”—the ability to pause before reacting. This makes the emotional response impulsive and immediate.
- Autism: Here, the cause is often sensory sensitivities. When a brain is bombarded by lights, sounds, and social cues it cannot easily interpret, it reaches a state of “sensory overload,” leading to a meltdown that is purely biological in nature.
- BPD and PTSD: In borderline personality disorder and complex PTSD, the dysregulation is often a survival mechanism. The brain has been “trained” by trauma to react with maximum intensity to any perceived threat or rejection.
Signs and Symptoms of Emotional Dysregulation
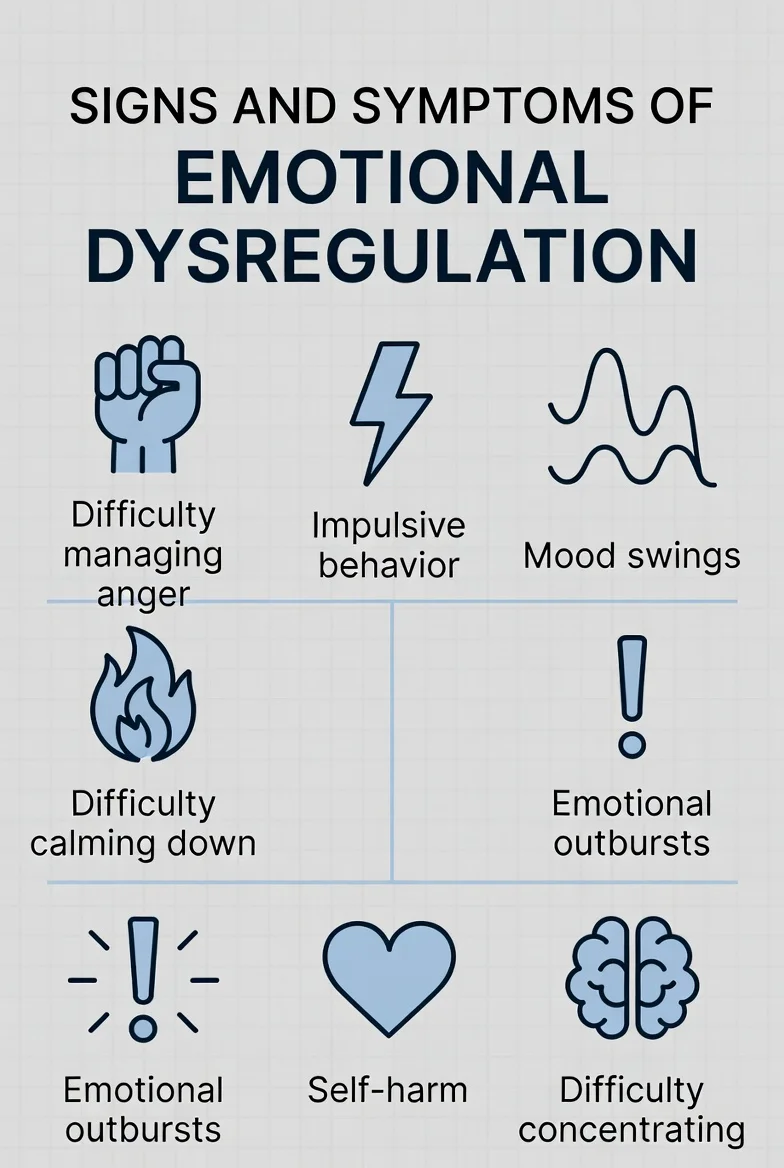
If you are wondering what emotional dysregulation looks like, it is helpful to look for the “Three I’s”: Intensity, Impulsivity, and Inability to calm down.
Behavioral Manifestations
In children, this often looks like screaming, throwing objects, or “shutting down” entirely when frustrated. In adults, it can be more subtle but equally destructive. An adult might experience the following:
- Sudden Irritability: Snapping at colleagues or family over small errors.
- Rapid Mood Changes: Moving from high energy to deep depression within hours.
- Social Withdrawal: Leaving an event abruptly because of an internal emotional surge that feels “too big” to handle.
The ADHD/Autism “Flavor” of Symptoms
Emotional dysregulation and ADHD symptoms often include “flash anger” that disappears as quickly as it arrived, leaving the individual confused by the damage they caused while angry. In autism, you might see “stimming” (repetitive movements) increase as the person tries to regulate a nervous system that feels like it’s vibrating.
In my years of practice, I have observed a nuance that many overlook: the role of circadian rhythms. I once worked with a patient, “Mark,” who was convinced he had a personality disorder because of his nighttime rage. Through careful tracking, we realized his dysregulation only peaked when his sleep hygiene failed. When the brain is sleep-deprived, the prefrontal cortex essentially “goes offline,” leaving the emotional centers completely unchecked. For Mark, fixing his sleep was the “medication” that finally stabilized his mood.
Types of Emotional Dysregulation Disorders
It is vital to distinguish between situational stress and types of emotional dysregulation disorders. While anyone can become dysregulated under extreme pressure, certain conditions make it a chronic state.
a. Neurodevelopmental (ADHD and Autism)
In these cases, the dysregulation is “bottom-up.” The brain’s hardware is wired for high sensitivity and low inhibition. It is not a “mood disorder” in the traditional sense but a byproduct of how the brain processes information and stimulation.
b. Personality and Trauma-Based (BPD and C-PTSD)
Emotional dysregulation disorder vs. BPD is a common point of confusion. BPD is characterized by a pervasive pattern of instability in relationships and self-image, with emotional dysregulation as its core engine. In C-PTSD, the dysregulation is a “protective” response to past trauma, where the brain treats every disagreement as a life-or-death situation.
c. Mood-Related (DMDD and Bipolar)
Disruptive Mood Dysregulation Disorder (DMDD) is a diagnosis typically given to children who exhibit persistent irritability and frequent, severe physical outbursts. In bipolar disorder, the dysregulation occurs in distinct cycles (mania or depression), whereas in ADHD, the shifts are often momentary and triggered by external events.
| Type | Primary Trigger | Duration of Episode |
| ADHD | Frustration / Rejection | Minutes to Hours |
| BPD | Interpersonal Slights | Hours to Days |
| Autism | Sensory Overload | Variable (until reset) |
| C-PTSD | Trauma Reminders | Variable |
Emotional Dysregulation in Relationships
Perhaps the most painful aspect of being unable to regulate emotions is the toll it takes on loved ones. Relationships require a “co-regulation” dance; when one partner is constantly out of step, the other often feels they are “walking on eggshells.”
Conflict Escalation and Withdrawal
I often see a pattern in my office where a minor disagreement turns into a “scorched earth” argument. Because the dysregulated partner feels emotions so intensely, they may use “all-or-nothing” language (“You never help me!” or “I’m leaving!”). When the surge passes, they feel immense shame, but the partner is left with the emotional shrapnel.
Strategies for Couples
To mitigate this, I teach couples the “20-Minute Rule.” If one person feels their “logical brain” slipping away, they call a timeout. This isn’t a “silent treatment”; it is a clinical necessity to allow the nervous system to return to a baseline before the conversation continues.
Assessment and Testing
If you recognize these patterns, an emotional dysregulation test can provide clarity. In a professional setting, we use tools like the DERS (Difficulties in Emotion Regulation Scale) or specific ADHD assessments.
Testing helps us understand if your dysregulation is “top-down” (thinking patterns) or “bottom-up” (biological/sensory). For parents, seeing these results can be a relief—it proves that their child isn’t “being bad” but is instead dealing with a measurable clinical challenge.
Treatment and Management
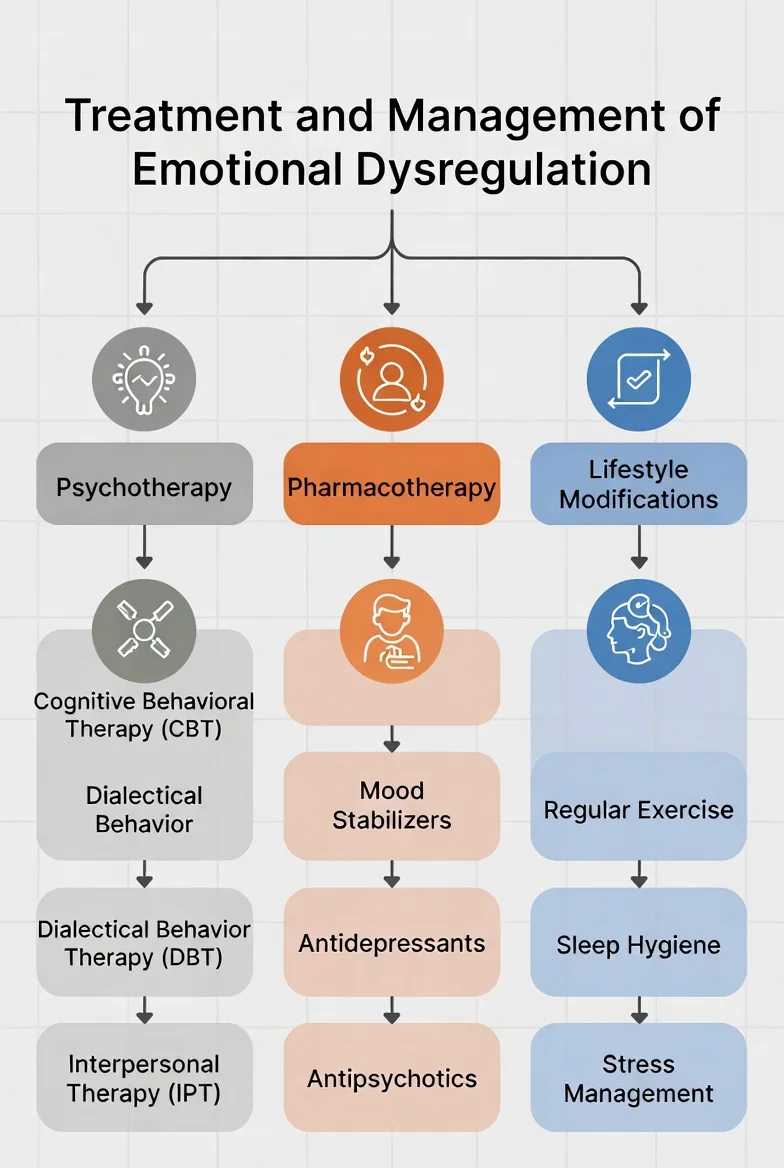
The most encouraging news I share in my clinic is that the brain is capable of remarkable neuroplasticity. You can literally “re-wire” how your brain handles emotional surges.
How to treat emotional dysregulation involves a multi-pronged approach: strengthening the “logical brakes,” lowering the “emotional alarm,” and managing the biological “engine.”
Therapeutic Interventions
In my practice, I have seen that “talk therapy” alone is often insufficient for dysregulation because you cannot “talk” your way out of a physiological hijack. Instead, we use skills-based approaches:
- Dialectical Behavior Therapy (DBT): This is the gold standard for how to fix emotional dysregulation. It teaches “distress tolerance”—how to survive a feeling without making things worse—and “emotion regulation” skills to reduce your vulnerability to the “emotional waves.”
- Cognitive Behavioral Therapy (CBT): We work to identify the “cognitive distortions” (like “catastrophizing”) that act as fuel for the emotional fire.
- Parent Coaching: For children, the treatment is often focused on the parents. We teach “co-regulation” techniques, where the parent uses their own calm nervous system to help settle the child’s “storm.”
Medication Management
When the “biological volume” is too loud, medication for emotional dysregulation can provide a necessary floor of stability.
| Medication Category | Primary Use in Dysregulation | How it Helps |
| Stimulants (e.g., Vyvanse) | ADHD-related dysregulation | Strengthens the “brakes” (prefrontal cortex). |
| Non-Stimulants (e.g., Guanfacine) | High-arousal / Rejection sensitivity | Lowers the “fight or flight” response |
| SSRI/SNRIs | Comorbid Anxiety/Depression | Raises the “threshold” for emotional triggers |
| Mood Stabilizers | Bipolar / Severe Volatility | Smooths out the “peaks and valleys” of mood |
Practical Daily Strategies
To improve your emotional regulation, you must practice when you are calm. You cannot learn to swim during a hurricane.
- The 90-Second Rule: A chemical emotional surge only lasts about 90 seconds. If you can use deep breathing or cold water on your face to “ride the wave” for that minute and a half, the intensity will naturally drop.
- Emotion Labeling: Use emotion regulation worksheets or journals to name exactly what you feel. Moving a feeling from “vague distress” to “I feel overlooked” engages the logical brain.
- Sensory Resets: Especially for those with autism-related dysregulation, having a “sensory toolkit” (weighted blankets and noise-canceling headphones) can prevent a meltdown before it starts.
I recall a patient, “Sarah,” who struggled with extreme emotional dysregulation in her relationships. Every minor critique from her partner felt like a soul-crushing rejection.
Through a combination of DBT skills and optimizing her circadian rhythms, she learned to “catch the spark” before the fire started. A year later, she shared that for the first time in her life, she felt she was the “driver” of her emotions rather than the “passenger.”
Frequently Asked Questions
Can emotional dysregulation in children improve naturally with age?
While the prefrontal cortex naturally matures until the mid-20s, children with ADHD or trauma often require targeted support. They don’t just “grow out of it”; they must learn the skills to manage their unique neurobiology.
Is emotional dysregulation a symptom of ADHD or autism?
Yes, it is incredibly common in both. In ADHD, it is driven by impulsivity and executive dysfunction. In autism, it is often driven by sensory overload and difficulty with social-emotional processing.
How do I know if I have emotional dysregulation as an adult?
If you feel your emotions are “too big” for the situation, if you take a long time to “come down” after being upset, or if your moods are negatively impacting your work and marriage, you likely meet the criteria for dysregulation.
Can therapy alone fix emotional dysregulation?
For many, yes. Skills-based therapies like DBT are incredibly effective. However, if the cause is deeply biological (like severe ADHD), a combination of therapy and medication usually yields the best results.
Are medications always needed?
Not always. Many people find success through lifestyle changes, therapy, and mindfulness. Medication is typically considered when dysregulation is so severe that the individual cannot “access” their therapy skills because they are constantly in a state of crisis.
Conclusion
Living with emotional dysregulation is exhausting, but it is not a life sentence. Your “big feelings” are often the flip side of a high capacity for empathy, creativity, and passion. The goal of treatment isn’t to turn off your emotions but to give you the steering wheel so you can choose where those emotions take you.
If you or your child is struggling, start with a professional evaluation. You deserve to live a life that isn’t dictated by the next “storm.”
References
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.