Fluoxetine (Prozac): A Comprehensive Guide to Uses, Mechanism, and Safety

In my practice as a clinical psychologist, I often work with individuals who feel as though they are wading through a thick, gray fog—the hallmark of major depression—or those trapped in the exhausting “hamster wheel” of obsessive-compulsive thoughts.
When a psychiatrist or primary care physician suggests fluoxetine, better known by its original fluoxetine brand name, Prozac, it often marks a turning point in the therapeutic journey.
Fluoxetine was the first selective serotonin reuptake inhibitor (SSRI) to gain widespread global recognition, and for good reason.
It is a versatile “workhorse” in mental health, offering a bridge for patients to re-engage with their lives. However, the path to stabilization isn’t always immediate.
Many of my patients report noticeable improvements in mood and a reduction in the “sharp edges” of anxiety after 2 to 4 weeks, though I always counsel them that reaching a full therapeutic “steady state” can take up to 8 weeks.
Understanding what fluoxetine is and how it interacts with your biology is essential for managing expectations and achieving long-term wellness.
What is Fluoxetine Used For?
While many categorize it simply as an “antidepressant“, the list of fluoxetine uses is remarkably diverse, reflecting its ability to stabilize various neural pathways.
FDA-Approved Indications for Humans
- Major Depressive Disorder (MDD): The primary use is for lifting a persistent low mood and increasing energy.
- Obsessive-Compulsive Disorder (OCD): Fluoxetine helps reduce the intensity of intrusive thoughts and the urge to perform repetitive compulsions.
- Panic Disorder: It is effective in reducing the frequency and severity of sudden panic attacks.
- Bulimia Nervosa: Fluoxetine is uniquely FDA-approved to help reduce binge-eating and purging behaviors.
- Premenstrual Dysphoric Disorder (PMDD): Often prescribed in lower doses or intermittently to manage severe emotional distress related to the menstrual cycle.
Veterinary Applications: Fluoxetine for Dogs and Cats
An interesting facet of this medication is its cross-species utility. In veterinary medicine, fluoxetine for dogs is frequently used to treat separation anxiety and certain types of aggression.
Similarly, fluoxetine for cats can be a lifesaver for managing house-soiling (urine marking) or compulsive over-grooming caused by stress.
Just as in humans, the medication helps “lower the volume” on the animal’s fight-or-flight response.
In my clinical observations, whether a patient is taking fluoxetine 20 mg for depression or a higher dose for OCD, the goal is the same: restoring a sense of agency over one’s emotional life.
How Fluoxetine Works
To understand how fluoxetine works, we have to move beyond the simplistic “chemical imbalance” theory and look at the sophisticated way it modulates brain communication. Fluoxetine is the quintessential SSRI, but its impact on the brain is multifaceted.
The Synaptic “Cleaning” Process (Substance over Fluff)
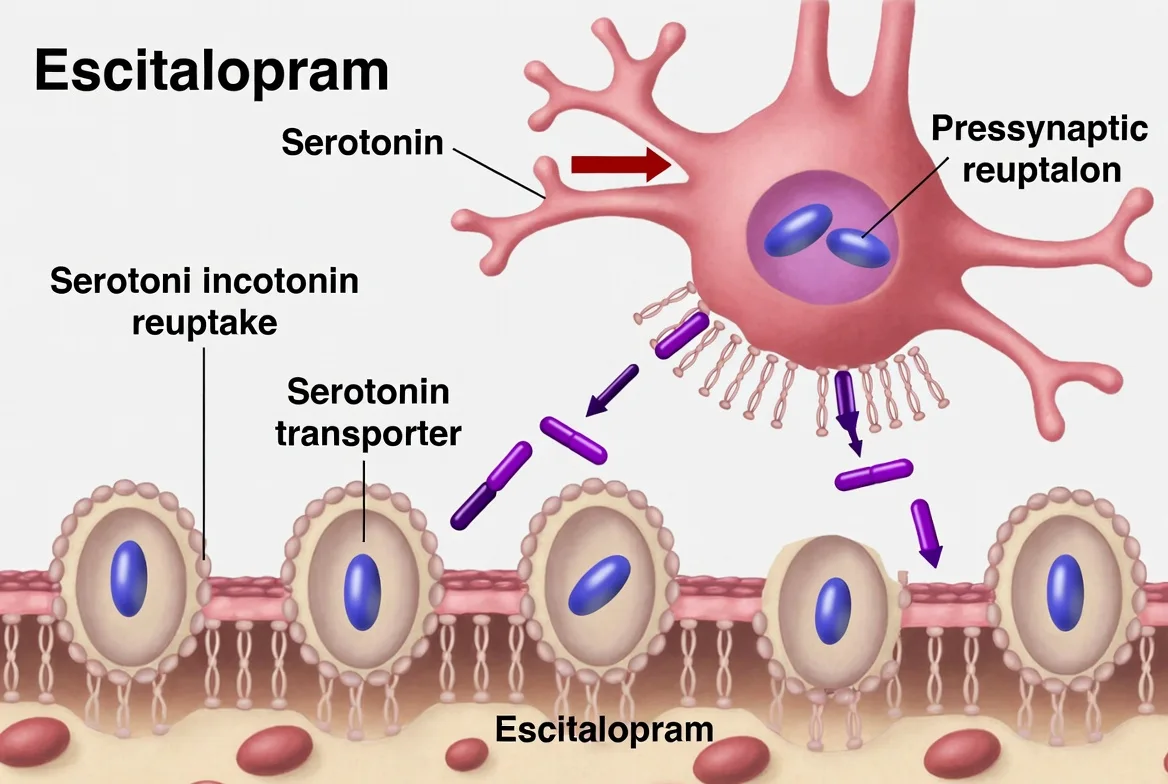
In a brain struggling with depression or anxiety, serotonin—a neurotransmitter responsible for mood, sleep, and emotional processing—is often reabsorbed too quickly by the sending neuron. This leaves the receiving neuron “thirsty” for a signal that never fully arrives.
- Selective Reuptake Inhibition: Fluoxetine blocks the “reuptake” pump (the serotonin transporter). By doing this, it forces serotonin to linger longer in the synaptic cleft—the tiny space between brain cells.
- Downregulation of Receptors: The “Why” behind the 4-to-8-week delay in feeling better isn’t just about the serotonin levels themselves. When serotonin stays in the synapse longer, the brain eventually responds by “downregulating” or desensitizing certain receptors. This long-term structural change is often when patients finally feel the “fog” lifting.
- Neuroplasticity and BDNF: Newer research suggests that fluoxetine increases the production of brain-derived neurotrophic factor (BDNF). Think of BDNF as “fertilizer” for the brain. It encourages neuroplasticity, helping the brain repair damaged connections and grow new ones in the hippocampus, an area vital for mood regulation and memory.
The Pharmacokinetic “Safety Net”
What sets fluoxetine apart from other SSRIs like sertraline (Zoloft) or paroxetine (Paxil) is its exceptionally long half-life.
- The Parent Drug: Fluoxetine stays in your system for about 2 to 4 days.
- The Active Metabolite: Its byproduct, norfluoxetine, can stay in your system for 7 to 15 days.
This long duration acts as a built-in safety net. If a patient accidentally misses a dose, they are much less likely to experience the “brain zaps” or sudden irritability common with shorter-acting meds. This slow “washout” also makes fluoxetine the easiest SSRI to taper off of when the time is right.
A nuance I often observe is that fluoxetine is more “activating” than other SSRIs. While some medications make you sleepy, fluoxetine tends to provide a slight boost in energy and focus.
The Nuance: I once worked with a patient, “Sarah,” who struggled with “leaden paralysis”—a type of depression where her limbs felt like they weighed a thousand pounds.
Because fluoxetine has a slightly stimulating effect on certain dopamine and norepinephrine receptors in the prefrontal cortex, it helped her regain her executive function. However, because of this “spark”, I always recommend taking it in the morning.
Taking it at night can interfere with circadian rhythms, leading to insomnia that mimics anxiety.
Dosing and Administration

The fluoxetine dosage is highly individualized, often starting at the lowest dose of fluoxetine to minimize initial side effects.
- Standard Starting Dose: Usually fluoxetine 20 mg per day for depression or anxiety.
- OCD and Bulimia: These conditions often require higher doses, sometimes moving up to fluoxetine 60 mg or even 80 mg to achieve a therapeutic effect.
- Panic Disorder: Clinicians often start even lower, at fluoxetine 10 mg, because patients with panic disorder can be hypersensitive to the initial “jittery” feeling the medication may cause.
Administration Tips
I advise my patients to take their capsule or tablet with breakfast. While it can be taken without food, a small meal helps mitigate the mild nausea that some experience in the first week. If you are using the liquid form (often used for children or elderly patients), precision in measurement is key.
Side Effects and Safety
No medication is without trade-offs. While fluoxetine is generally well-tolerated, being prepared for the “adjustment phase” is vital for staying the course.
Common Side Effects
Most side effects are “front-loaded,” meaning they appear in the first two weeks and then fade as the brain adapts.
- Gastrointestinal: Nausea or “loose stools” (the gut is lined with serotonin receptors).
- Sleep Changes: Insomnia or vivid dreams.
- Initial Jitteriness: A temporary increase in “nervous energy.”
Specific Concerns: Weight and Sex
- Does fluoxetine cause weight gain? Compared to other antidepressants, fluoxetine is actually considered weight-neutral or may even cause slight weight loss initially due to appetite suppression.
- Sexual Side Effects: Both men and women may notice a decrease in libido or a delay in reaching orgasm. This is a common fluoxetine side effect in females that should be discussed openly with a provider, as dose adjustments or “add-on” medications can often help.
Jason (anonymized) was a high-level executive treated for panic disorder. When he started fluoxetine 10 mg, he called me on day three, panicking because he felt “electrified” and couldn’t sleep. He wanted to quit immediately.
We used a cognitive-behavioral intervention to reframe these sensations. Instead of “I am having a panic attack,” we labeled it as “My brain is adjusting to its new fuel.” We shifted his dose to 7:00 AM and added a 10-minute morning mindfulness practice to “ground” the extra energy.
By day ten, the jitters vanished, and by week six, Jason reported his first panic-free month in three years. His story is a testament to the fact that the first week on an SSRI is often the hardest, but the reward for persistence is profound.
Onset of Action and Duration in the Body
The most frequent question I receive after a prescription is written is “How long does fluoxetine take to work?” Unlike a pain reliever that acts in thirty minutes, an SSRI requires a fundamental shift in how your brain’s receptors respond to neurochemicals.
The Clinical Timeline of Recovery
In my practice, I find that patients often experience a “staggered” recovery. It is rare for everything to improve at once.
- Days 7 to 14: You may notice small, objective changes before your mood actually lifts. Patients often report better sleep quality or a slight return of appetite. Friends or family might notice the patient is more talkative or making more eye contact.
- Weeks 2 to 4: This is typically when the “emotional blunting” or heavy sadness begins to thin. You might find you have more energy to complete daily tasks—a sign that your executive function is beginning to come back online.
- Weeks 4 to 8: This is the window for the “full therapeutic effect.” For complex conditions like OCD or Bulimia, it truly takes the full two months for the brain to reach a stable, new equilibrium.
Why Fluoxetine Stays in Your System
As mentioned, the fluoxetine half-life is the longest in its class. This has a profound impact on how the drug behaves if you stop taking it.
- The “Self-Tapering” Effect: Because the active metabolite norfluoxetine stays in the blood for up to two weeks, the drug naturally leaves your body very slowly.
- Missed Doses: If you forget a Saturday dose of fluoxetine 20 mg, you likely won’t feel a difference on Sunday because your blood levels remain high.
- Washout Period: If a clinician needs to switch you to a different class of medication, like an MAOI, you must wait at least five weeks after your last dose of fluoxetine to ensure it is completely out of your system to avoid serotonin syndrome.
Weight Changes and Metabolic Effects
A significant source of anxiety for my patients is the question, “Does fluoxetine cause weight gain?” There is a persistent myth that all antidepressants lead to rapid weight gain, but the data on fluoxetine tells a more nuanced story.
Weight Loss vs. Weight Gain
| Phase of Treatment | Typical Weight Impact | Clinical Reason |
| Initial (0–3 Months) | Possible Weight Loss | Mild nausea and appetite suppression. |
| Maintenance (6+ Months) | Weight Neutral | Appetite returns to a healthy baseline. |
| Long-Term (1 Year+) | Possible Mild Gain | Often reflects “recovery weight” from a depressive state. |
In my experience, whether fluoxetine causes weight gain or loss depends largely on the individual’s baseline.
Some patients lose weight because they stop “emotional eating” once their anxiety is managed. Others gain a few pounds because their depression-related lack of appetite resolves, and they finally enjoy food again.
Compared to medications like paroxetine (Paxil) or mirtazapine (Remeron), fluoxetine is considered one of the most “metabolically friendly” antidepressants available in 2026.
Precautions, Contraindications, and Safety
While fluoxetine is exceptionally safe for most, there are “red flag” interactions that require professional vigilance.
Fluoxetine and Alcohol
One of the most common questions is about fluoxetine and alcohol. In my practice, I generally advise a “low-to-no” approach.
- Increased Sedation: Alcohol is a depressant, and combining it with an SSRI can lead to extreme drowsiness and impaired judgment.
- The “Next Day” Slump: Alcohol temporarily spikes serotonin, but the “crash” the following day can counteract the stabilizing work the fluoxetine is trying to do.
Serious Risks: Serotonin Syndrome
While rare, serotonin syndrome is a medical emergency that occurs when there is too much serotonin in the brain. This usually happens when fluoxetine is combined with other “serotonergic” agents like St.
John’s Wort, certain migraine meds (triptans), or recreational drugs. Symptoms include high fever, agitation, increased heart rate, and tremors.
Frequently Asked Questions
Is fluoxetine the same as Xanax?
No. Xanax is a benzodiazepine used for immediate, short-term relief of acute anxiety. Fluoxetine is an SSRI used for long-term stabilization of mood and anxiety disorders.
Can you drink alcohol on fluoxetine?
It is generally discouraged. While a single glass of wine may be tolerated by some, heavy drinking can increase side effects and worsen depression symptoms.
Does fluoxetine make you tired?
While it can cause mild drowsiness in some, it is actually more likely to be “activating.” This is why taking fluoxetine 20 mg in the morning is the clinical standard.
What is fluoxetine 20 mg used for?
This is the “standard” dose for treating major depression, general anxiety, and PMDD.
How long does it take for fluoxetine to work?
You may feel small shifts in energy or sleep within 1 to 2 weeks, but the full antidepressant effect typically requires 4 to 8 weeks of consistent use.
Conclusion
Fluoxetine (Prozac) remains a cornerstone of modern psychiatry for a reason: it works, it is safe, and it is accessible. Increasing the “available” serotonin in your brain, it provides the biological support needed to engage in the hard work of therapy and lifestyle change.
If you are just beginning your journey with fluoxetine, remember that patience is your most important ally. The first few weeks of “jitters” or stomach upset are often just signs that your brain is recalibrating.
Work closely with your care team, prioritize your morning dose to protect your circadian rhythms, and give yourself the grace to heal on a biological timeline. You are not just taking a pill; you are investing in the pursuit of a healthier future.
References & Resources
- National Institute of Mental Health (NIMH): Mental Health Medications
- National Alliance on Mental Illness (NAMI): Fluoxetine (Prozac) Guide
- FDA.gov: Prozac (fluoxetine) Prescribing Information
- Bipolar Lives: Antidepressants and Mood Stabilizers
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.