Mood Stabilizers vs. Antipsychotics: Differences, Uses, and Which Is Better for Bipolar & BPD
Navigating the world of psychiatric medication can feel like learning a foreign language. For those diagnosed with bipolar disorder, borderline personality disorder (BPD), or severe depression, two terms frequently appear: mood stabilizers and antipsychotics. Often, these medications are prescribed for the same symptoms, leading many to wonder about the nuances of their labels.
This comprehensive guide explores the structural and functional differences between these two drug classes, helps clarify why the lines between them are increasingly blurred, and provides evidence-based insights into which may be better suited for specific mental health challenges in 2026.
Why People Confuse Mood Stabilizers and Antipsychotics
The confusion surrounding mood stabilizers vs. antipsychotics is not due to a lack of research, but rather a shift in how modern psychiatry treats symptoms. Historically, medications were named for their primary function: antipsychotics were for psychosis, and mood stabilizers were for the “highs and lows” of bipolar disorder.
However, the line between these classes has blurred significantly. Today, many “atypical antipsychotics” are FDA-approved as primary treatments for bipolar depression and maintenance. Furthermore, clinicians often prescribe both simultaneously to achieve “synergy.”
Are mood stabilizers and antipsychotics the same? Technically, no. They belong to different chemical families and interact with the brain through different pathways. However, in a real-world clinical setting, their roles overlap. This article will break down the “why” and “how” behind these prescriptions, helping you move past the labels to understand the actual medicine.
What Are Mood Stabilizers?
In psychiatric terms, a mood stabilizer is a medication used to treat mood disorders characterized by intense and sustained mood shifts. Their primary goal is to provide a “floor” and a “ceiling” to a person’s emotional range—preventing the devastating “lows” of depression and the dangerous “highs” of mania.
Core Mood Stabilizer Drugs for Bipolar
There are four primary medications traditionally categorized as mood stabilizers:
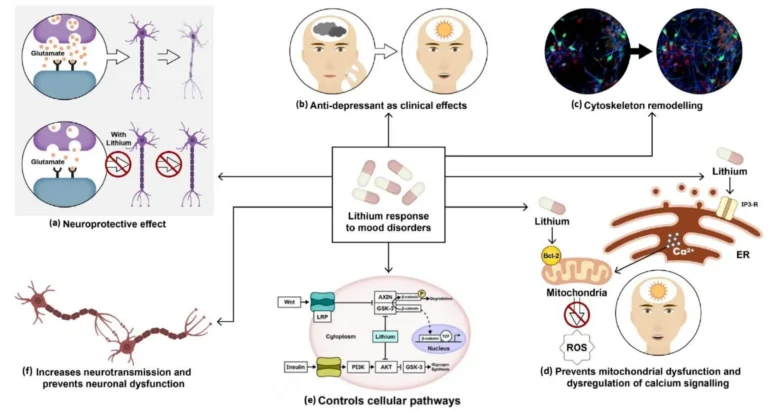
- Lithium: The “gold standard” for bipolar I disorder. It is a naturally occurring salt that remains one of the most effective treatments for preventing suicide and manic relapse.
- Valproate (Depakote): An anticonvulsant that is particularly effective for “rapid cycling” bipolar disorder and mixed episodes.
- Carbamazepine (Tegretol): Another anticonvulsant often used when lithium or valproate is not tolerated.
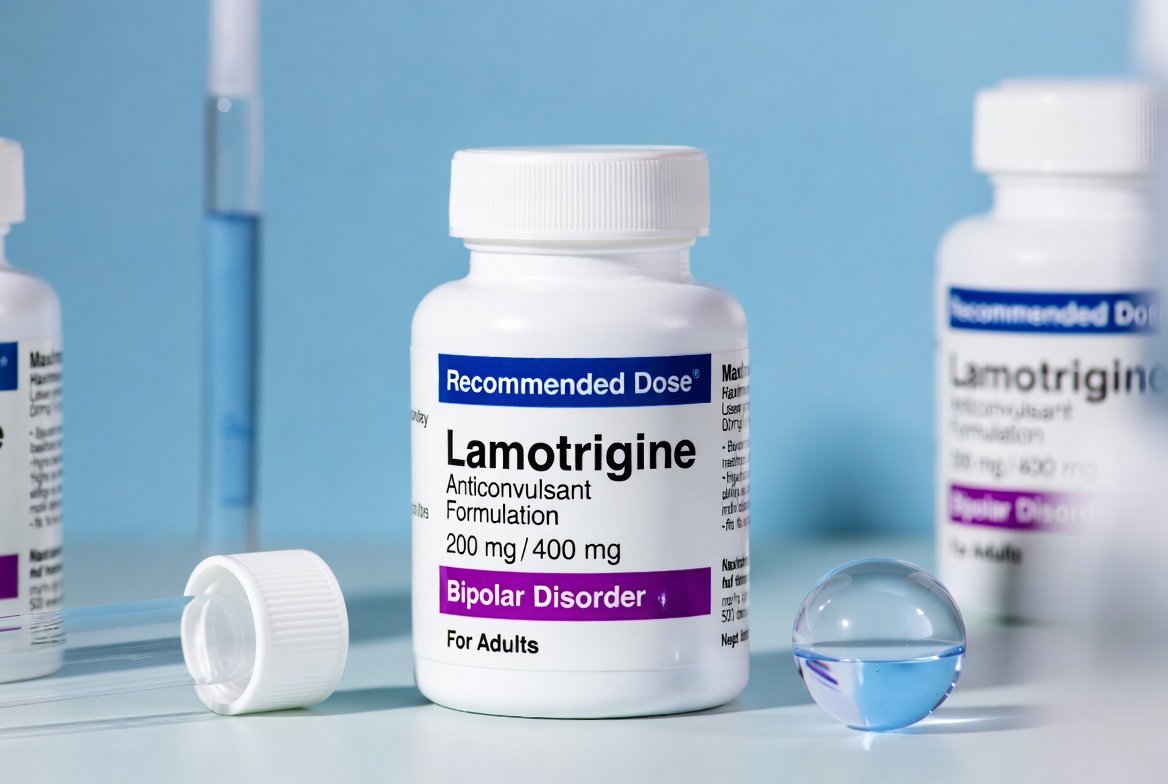
- Lamotrigine (Lamictal): Unique among stabilizers because it is significantly more effective at preventing the “lows” of bipolar depression than the “highs” of mania.
What Mood Stabilizers Treat Well
Mood stabilizers excel at long-term maintenance. They are designed to be taken over the years to keep the brain’s chemistry within a stable “window.” While they are excellent at preventing future episodes, they are often slower to act during an acute crisis—such as active psychosis or extreme agitation—than antipsychotics.
You may be interested in reading about best bipolar disorder tracking app.
What Are Antipsychotics?
Antipsychotics were originally developed to treat schizophrenia by reducing “positive symptoms” like hallucinations and delusions. However, their role has expanded massively.
Typical vs. Atypical Antipsychotics
- Typical (First-Generation): Older drugs like Haloperidol. They are powerful but often carry a high risk of movement-related side effects (extrapyramidal symptoms).
- Atypical (Second-Generation): Modern drugs like Quetiapine (Seroquel), Aripiprazole (Abilify), and Olanzapine (Zyprexa). These are the versions most commonly used for mood stabilization.
Why Antipsychotics Work for Mood Stabilization
Atypical antipsychotics don’t just block dopamine; they also modulate serotonin. This dual action allows them to act as “mood stabilizers” in their own right. They are often preferred in acute situations because they work much faster than traditional stabilizers. If someone is in the middle of a manic crisis, an antipsychotic can often “bring them down” within days, whereas lithium might take weeks to reach therapeutic levels.
Mood Stabilizers vs. Antipsychotics
Understanding the difference between mood stabilizers and antipsychotics requires looking at their “mechanics” and “timelines.”
Primary Mechanism of Action
- Mood Stabilizers: Generally work by altering ion transport (like sodium or calcium) across cell membranes or by enhancing GABA (a calming neurotransmitter). They essentially “quiet” overactive electrical signals in the brain.
- Antipsychotics: Primarily target dopamine receptors (specifically D2) and serotonin receptors (5-HT2A). They act as “chemical dampers” on the neurotransmitters that drive racing thoughts and sensory distortions.
Speed and Purpose
Antipsychotics are the “firefighters”—they are excellent for putting out the immediate fire of mania or severe depression. Mood stabilizers are the “architects”—they work slowly to build a structure that prevents the fire from starting in the first place.
Side Effect Profiles
This is often where patients make their choice.
- Mood Stabilizers: Often require blood monitoring (especially Lithium and Valproate) to ensure levels aren’t toxic. Common side effects include tremors, thirst, and potential impacts on thyroid or kidney function.
- Antipsychotics: Carry a higher risk of metabolic side effects, including weight gain, increased blood sugar, and sedation.
Comparison Table: At a Glance
| Feature | Mood Stabilizers | Atypical Antipsychotics |
| Primary Goal | Relapse prevention / Stability | Acute symptom control / Depression |
| Speed of Onset | Slow (Weeks) | Fast (Days) |
| Main Target | Ion channels / GABA | Dopamine / Serotonin |
| Common Drugs | Lithium, Lamictal, Depakote | Seroquel, Abilify, Latuda |
| Blood Tests? | Often required | Rarely required (Metabolic checks instead) |
Are Mood Stabilizers and Antipsychotics the Same?
The short answer is no, but they are often used for the same destination.
Think of it like heart health: you might be prescribed a beta-blocker (to slow the heart rate) or a statin (to manage cholesterol). They are different types of medicine, but they are both “heart medications” working toward a healthy cardiovascular system.
In psychiatry, antipsychotics can act as mood stabilizers, but most mood stabilizers cannot act as antipsychotics. For example, Lithium will not stop someone from hearing voices or experiencing a complex delusion as effectively as an antipsychotic will. However, Seroquel can stabilize a mood just as effectively as Lithium in many patients. This asymmetrical relationship is why many patients end up on an antipsychotic even if they have never experienced a “psychotic” symptom.
Mood Stabilizers vs. Antipsychotics for Bipolar Disorder
When treating bipolar disorder, the choice between these classes depends on the “state” of the patient.
For Acute Mania
Antipsychotics are usually the first line of defense. Because mania involves a surge of dopamine and physical agitation, the “dampening” effect of an antipsychotic like Risperidone or Olanzapine is often necessary to ensure the patient’s safety and return to reality quickly.
For Bipolar Depression
This is where atypical antipsychotics have seen the most growth. Drugs like Quetiapine (Seroquel) and Lurasidone (Latuda) are specifically FDA-approved for bipolar depression, whereas many traditional mood stabilizers (with the exception of Lamictal) are not as strong in the “depressive pole.”
For Maintenance (Relapse Prevention)
Traditional mood stabilizers, particularly Lithium, are the gold standard here. They have decades of data proving their ability to keep patients stable for 10, 20, or 30 years with fewer metabolic complications than long-term antipsychotic use.
The Case for Combination Therapy
Many people take both. A common regimen might include Lithium (for long-term stability) and Seroquel (to help with sleep and depressive symptoms). This “cocktail” approach allows clinicians to use lower doses of each, potentially minimizing the side effects of both.
Best Antipsychotics for Bipolar I vs. Bipolar II
While both Bipolar I and II involve cycling moods, the “target” for medication often shifts depending on which type you are treating.
Bipolar I: Managing the “Highs”
In Bipolar I, the primary danger is often acute mania, which can include psychosis, severe agitation, and hospitalization.
- First-Line Needs: Medications that act quickly on dopamine D2 receptors are preferred.
- Examples: Olanzapine (Zyprexa) and Risperidone (Risperdal) are the heavy hitters. They are highly effective at “braking” a manic episode within 24 to 48 hours.
- Mixed Episodes: If you experience mania and depression simultaneously, Cariprazine (Vraylar) is a modern choice that has shown high efficacy for these complex “mixed” states.
Bipolar II: Managing the “Lows”
Bipolar II is dominated by hypomania (which is often less disruptive) and debilitating, long-lasting depression.
- First-Line Needs: In this case, clinicians prioritize medications with high serotonin (5-HT) activity to “lift” the mood without triggering a switch into hypomania.
- Examples: Quetiapine (Seroquel) and Lurasidone (Latuda) are the gold standards. Lumateperone (Caplyta) is also a 2026 favorite for Bipolar II due to its minimal side effect profile.
Is Seroquel a Mood Stabilizer or Antipsychotic?

This is one of the most common questions in psychiatry. Officially, Seroquel (quetiapine) is an atypical antipsychotic. However, because it is one of the only drugs FDA-approved for both bipolar mania and bipolar depression (as well as maintenance), many doctors and patients refer to it as a mood stabilizer.
In the 2026 clinical landscape, Seroquel is often described as a “multifunctional” agent because its effects change dramatically depending on the dosage. Unlike traditional mood stabilizers like Lithium, which primarily manage ion channels, Seroquel targets a complex web of dopamine, serotonin, and norepinephrine receptors.
The “Three-in-One” Drug
Seroquel’s versatility comes from its primary active metabolite, norquetiapine. While quetiapine itself manages dopamine, norquetiapine acts like a potent antidepressant by inhibiting the norepinephrine transporter (NET). This “dual action” is why Seroquel can treat a manic “high” and a depressive “low” using the same molecule.
- The “Antipsychotic” side: At high doses (400–800mg), quetiapine achieves high occupancy of dopamine D2 receptors. This is the range required to treat acute mania, hallucinations, or the “positive” symptoms of schizophrenia.
- The “Mood Stabilizer” side: At moderate doses (300mg), the focus shifts toward its antidepressant properties. Norquetiapine and serotonin (5-HT1A) agonism work together to lift bipolar depression, often outperforming traditional antidepressants without the risk of “switching” into mania.
- The “Sedative” side: At low doses (25–100mg), Seroquel acts almost exclusively as a potent antihistamine (H1 receptor blocker). While it is widely used off-label for insomnia, medical guidelines in 2026 strongly warn against this for the general population. Even at “sleep doses,” Seroquel can cause significant weight gain and metabolic changes that safer sleep aids avoid.
Is Abilify a Mood Stabilizer or Antipsychotic?
Officially, Abilify (aripiprazole) is classified as a third-generation atypical antipsychotic (Kirino, 2014; Kowalczyk et al., 2024). However, it is frequently utilized for mood stabilization due to its unique ability to regulate the dopamine and serotonin systems (Bhattacharjee & El-Sayeh, 2008).
The “Dopamine Thermostat”
Unlike many older antipsychotics that act as full antagonists—essentially “blocking” dopamine receptors—Abilify is a dopamine D2 receptor partial agonist (Kirino, 2014; Tuplin & Holahan, 2017).
This mechanism allows it to act like a thermostat for the brain:
- In high-dopamine states (Mania), it competes with endogenous dopamine to lower overall activity (Shim et al., 2007).
- In low-dopamine states (Depression), it provides a low level of “tonic” activity (approximately 25% to 30% of maximal dopamine activity), which can help lift mood (Bhattacharjee & El-Sayeh, 2008; Cookson & Pimm, 2021).
Use in Bipolar Disorder
Abilify is FDA-approved for several roles in bipolar I disorder, including the treatment of acute manic or mixed episodes and long-term maintenance therapy to prevent relapses (Mohr et al., 2022; StatPearls, 2023). Because it stabilizes rather than completely shuts down dopamine signaling, it is often referred to as a “dopamine system stabilizer” (Kirino, 2014).
The “Activating” Effect and Akathisia
One of the most distinct clinical features of Abilify is its “activating” or energizing quality. Because it maintains some level of dopamine activity, many patients find it less sedating than other antipsychotics like Seroquel or Zyprexa (Mohr et al., 2022).
However, this same stimulating effect can lead to specific side effects:
- Akathisia: This is a common adverse reaction characterized by an intense feeling of inner restlessness and an irresistible urge to move (Agarkar et al., 2013). Clinical trials show that akathisia occurs more frequently with Abilify than with a placebo, affecting approximately 10% to 15% of adult patients (FDA, 2011; Rosack, 2003).
- Insomnia and Restlessness: Its activating nature can also lead to difficulty sleeping or a general sense of agitation during the initial weeks of treatment (Cookson & Pimm, 2021).
Antipsychotics vs. Mood Stabilizers for BPD
Treating Borderline Personality Disorder (BPD) is fundamentally different because BPD is a personality disorder, not a primary mood disorder. As of 2026, there are no FDA-approved medications specifically for BPD. Instead, doctors use a “symptom-targeted” approach.
Symptom-Targeted Prescribing
- Antipsychotics for BPD: These are used to treat “cognitive-perceptual” symptoms, such as stress-induced paranoia or dissociation. Abilify and Olanzapine are common choices for reducing anger and impulsivity.
- Mood Stabilizers for BPD: Drugs like Lamotrigine are frequently used to help with “affective instability”—the rapid, hour-to-hour shifts in emotion that are hallmark to BPD.
Important Note: Clinical guidelines emphasize that Psychotherapy (specifically Dialectical Behavior Therapy or DBT) remains the primary treatment. Medication is viewed as a “supportive tool” rather than a cure.
Mood Stabilizers vs. Antidepressants: Where Antipsychotics Fit In
One of the most complex challenges in modern psychiatry is treating the depressive side of bipolar disorder without triggering a psychiatric emergency. While the instinct for many patients and general practitioners is to reach for a traditional antidepressant (like Prozac or Lexapro), this can often lead to unintended and severe consequences.
Understanding the “manic switch” and why antipsychotics have become the preferred “safety buffer” is essential for long-term stability.
The Danger of the “Manic Switch”
The primary risk in bipolar treatment is the “manic switch” caused by traditional antidepressants, particularly Selective Serotonin Reuptake Inhibitors (SSRIs) and Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs). In a bipolar brain, these medications can be “too effective” at boosting neurotransmitter levels.
Instead of simply returning the patient to a baseline “neutral” mood, the sudden influx of serotonin or norepinephrine can “propel” a bipolar brain into a dangerous manic or hypomanic state. This switch can manifest as:
- Rapid-Cycling: Moving quickly between emotional extremes.
- Mixed States: A particularly dangerous state where a patient feels the hopelessness of depression combined with the high energy and agitation of mania.
- Increased Suicidality: The physical energy provided by the antidepressant may return before the depressive thoughts vanish, giving a patient the “drive” to act on self-harming impulses.
The Antipsychotic Solution: Built-in Shields
Because of these risks, the 2026 clinical gold standard has shifted away from standalone antidepressants toward atypical antipsychotics. Medications like Latuda (lurasidone), Caplyta (lumateperone), and Vraylar (cariprazine) are now considered “first-line” for bipolar depression.
These drugs are often much safer than traditional antidepressants for several reasons:
- Dual-Action Properties: Unlike SSRIs, which primarily target serotonin, these antipsychotics modulate both dopamine and serotonin. This allows them to “lift” the mood (the antidepressant effect) while simultaneously “braking” excessive dopamine (the anti-manic effect).
- The Anti-Manic Shield: Because they occupy D2 dopamine receptors, they act as a “shield.” Even if the medication starts to push the mood upward, the antipsychotic component prevents the brain from crossing the threshold into full-blown mania.
- Combination Synergy: In cases where an antidepressant is necessary, clinicians almost always pair it with an antipsychotic or a mood stabilizer (like Lithium). The antipsychotic acts as an insurance policy, neutralizing the “switch” risk of the antidepressant.
Antipsychotics During Pregnancy: What’s Considered Safer?
In 2026, the mantra is “healthy mother, healthy baby.” Untreated bipolar disorder during pregnancy poses a high risk of relapse and postpartum psychosis.
- Risk-Benefit Framework: Doctors use the National Pregnancy Registry for Psychiatric Medications to track outcomes.
- Common Choices: Quetiapine (Seroquel) and Olanzapine have extensive data suggesting they are generally low-risk. Latuda is also frequently used.
- The Mood Stabilizer Comparison: Lithium is often more concerning due to a small risk of heart defects (Ebstein’s anomaly), making antipsychotics a preferred choice for many during the first trimester.
Mood Stabilizers vs. Antipsychotics for Anxiety Symptoms
It is a common misconception that mood stabilizers and antipsychotics are interchangeable with “anti-anxiety” meds like Xanax. In reality, their role in treating anxiety is indirect.
- Anxiety as a Symptom: In bipolar disorder, anxiety is often a “byproduct” of racing thoughts or depressive dread.
- Antipsychotics for Anxiety: Quetiapine (Seroquel) is the most studied for this purpose. At lower doses, it acts as a potent sedative and anxiolytic. However, the 2026 clinical consensus warns against using it as a primary anxiety treatment due to long-term metabolic risks.
- Mood Stabilizers for Anxiety: Medications like Valproate or Pregabalin (often used off-label) can help “quiet” the nervous system. Lamotrigine doesn’t treat acute panic but can reduce the “background noise” of chronic worry by stabilizing glutamate levels.
What Reddit Gets Right (and Wrong) About Mood Stabilizers vs. Antipsychotics
Searching mood stabilizers vs. antipsychotics on Reddit provides a raw look at the patient experience, but it requires a “filter.”
- The Lived Experience: Reddit is excellent for understanding the feeling of a medication—the “Seroquel hunger,” the “Abilify restlessness,” or the “Lithium thirst.”
- The Survivorship Bias: People who take Lithium for 20 years with zero issues rarely start a thread about it. You are mostly reading about people in the “trial and error” phase.
- The Misinformation: You may see users claiming “antipsychotics cause brain damage” or “mood stabilizers are just for seizures.” Clinical data from 2026 shows that when used correctly, these drugs are neuroprotective, actually preventing the brain matter loss associated with untreated manic episodes.
Frequently Asked Questions
Are mood stabilizers and antipsychotics the same?
No. Mood stabilizers (like Lithium) work on ion channels and GABA to prevent mood shifts. Antipsychotics (like Seroquel) work on dopamine and serotonin to control acute symptoms and psychosis.
Is Seroquel a mood stabilizer or an antipsychotic?
It is an atypical antipsychotic, but because it is so effective at stabilizing bipolar moods, it is frequently used as a primary mood stabilizer.
Is Abilify a mood stabilizer or an antipsychotic?
It is an atypical antipsychotic. It is unique because it “modulates” dopamine rather than just blocking it, making it less sedating for many people.
Which is better for bipolar disorder?
Neither is “better” in a vacuum. Antipsychotics are usually better for acute mania and bipolar depression, while traditional mood stabilizers (Lithium) are superior for long-term maintenance.
Can antipsychotics stabilize mood?
Yes. Modern “atypical” antipsychotics are highly effective at preventing both the highs and lows of bipolar disorder.
Conclusion
In the modern psychiatric landscape of 2026, the question isn’t which class is better, but which symptom profile you are trying to solve.
If your primary goal is to stop an acute manic episode or lift a heavy depression quickly, an atypical antipsychotic is likely your strongest ally. If you are looking for a lifelong “safety net” to prevent future episodes with minimal metabolic interference, a traditional mood stabilizer like Lithium or Lamictal may be the better foundation.
Most importantly, remember that these medications are tools, not labels. Work closely with your psychiatrist to tailor a “cocktail” that honors both your mental stability and your physical health.
Authoritative References
1. NICE(National Institute for Health and Care Excellence)
2. CANMAT(Canadian Network for Mood and Anxiety Treatments)
3. WFSBP (World Federation of Societies of Biological Psychiatry)
4. American Psychiatric Association (APA) – PsychiatryOnline
5. Journal of Clinical Medicine Research: BPD and Bipolar Overlap
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.