How Do Selective Serotonin Reuptake Inhibitors (SSRIs) Work? Mechanism, Benefits & Risks Explained
Have you ever wondered exactly what happens in your brain after you swallow that small capsule of sertraline or escitalopram? In my practice, I often meet patients who feel a mix of hope and hesitation when we discuss starting a prescription. They ask, How Do Selective Serotonin Reuptake Inhibitors (SSRIs) Work or “Will this change who I am?”
Understanding what selective serotonin reuptake inhibitors (SSRIs) are is the first step toward demystifying mental health treatment. While the term “chemical imbalance” is a common shorthand, the reality of how these medications interact with your neurons is far more fascinating.
These medications don’t just “add” serotonin; they change how your brain processes the joy and stability you already have. Let’s explore the clinical science behind the SSRI mechanism of action and what you can truly expect during treatment.
What Is Reuptake?
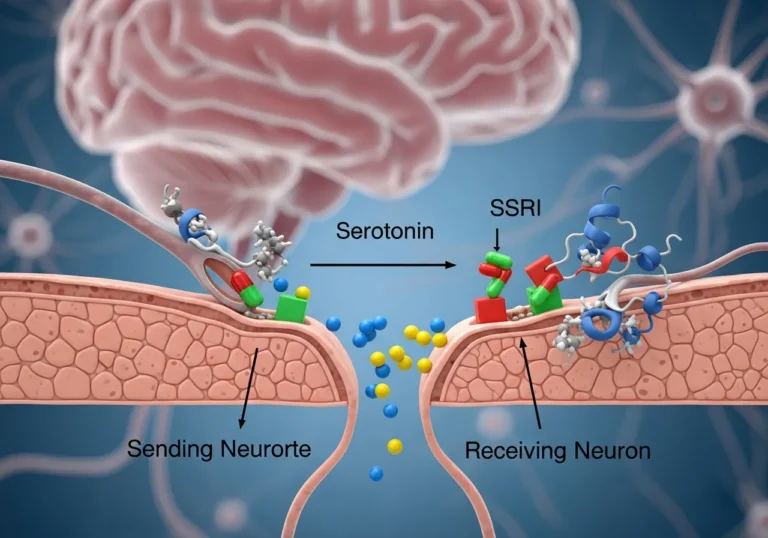
To understand how selective serotonin reuptake inhibitors work, we first have to look at the “synapse”—the tiny gap between your brain cells (neurons). Think of your neurons like two people standing on opposite sides of a canyon, tossing a ball (serotonin) back and forth to communicate.
In a healthy brain, the sending neuron releases serotonin into that gap. The serotonin then lands on the receiving neuron, delivering a message of “calm” or “safety.” However, the brain is also a master of recycling. Once the message is delivered, a protein called a reuptake transporter acts like a vacuum cleaner. It sucks the leftover serotonin back into the sending neuron to be used again later.
If that “vacuum cleaner” is too efficient, the serotonin doesn’t stay in the gap long enough to do its job. This is where a reuptake inhibitor is explained simply: it effectively “unplugs” the vacuum. By slowing down this recycling process, the medication ensures that more serotonin remains available to strengthen the signals between your cells.
How Do SSRIs Block Reuptake?
The SSRI mechanism of action is highly specific. Unlike older antidepressants that affected multiple chemicals at once, SSRIs are “selective.” They target the serotonin transporter (SERT) with surgical precision.
The Step-by-Step Biological Process
When you take an SSRI, the following sequence occurs within your neural pathways:
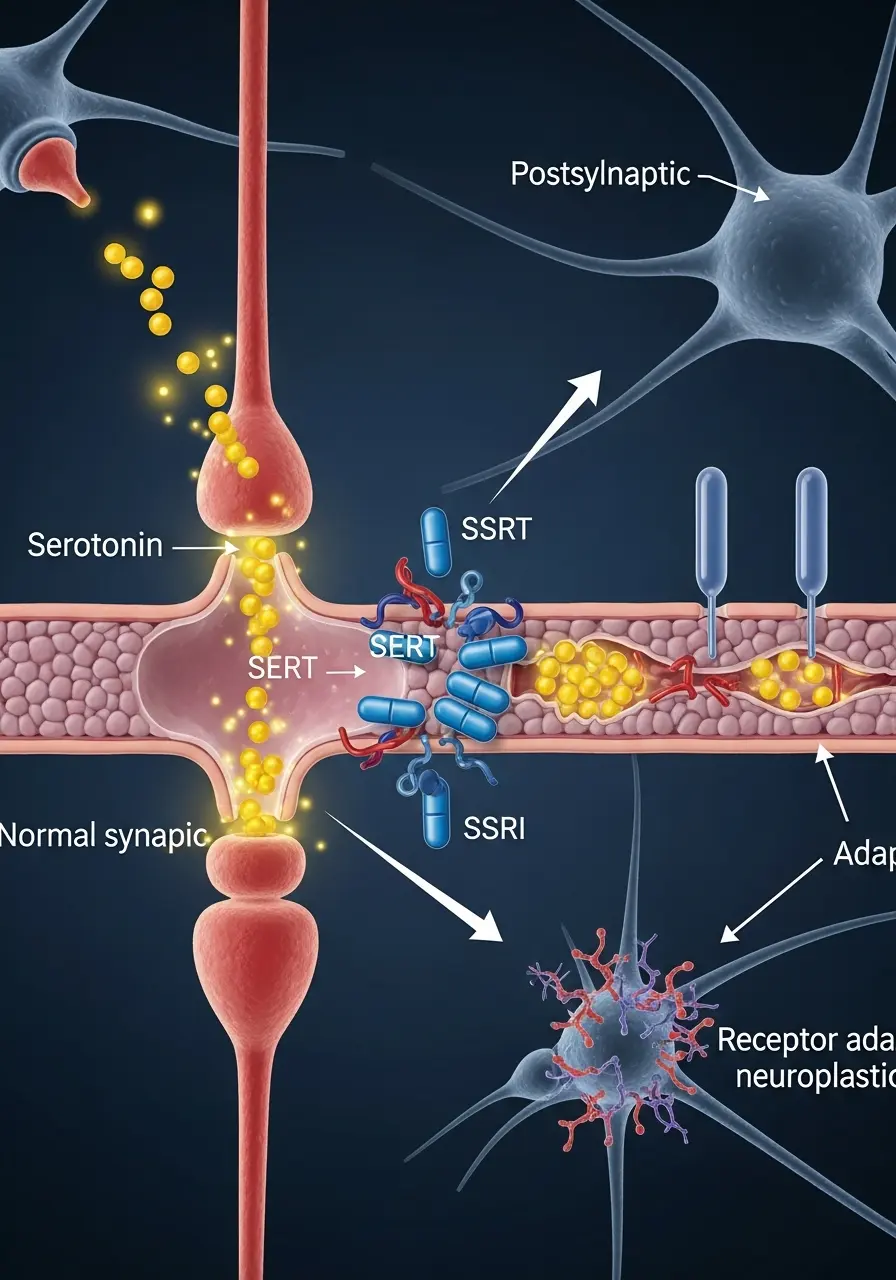
Step 01: Binding: The medication molecules travel to the presynaptic neuron and bind to the SERT proteins.
Step 02: Inhibition: This binding physically blocks the “doorway” that serotonin usually uses to re-enter the cell.
Step 03: Accumulation: Because the exit is blocked, serotonin builds up in the synaptic cleft (the gap).
Step 04: Receptor Adaptation: This is the most critical part. Over several weeks, the increased serotonin levels signal the receiving neuron to become more efficient. Your brain actually undergoes neuroplasticity, physically changing its receptor density to better manage your mood.
SSRI Mode of Action: A Visual Summary
- Step A: Serotonin is released into the synapse.
- Step B: SSRIs block the “reuptake pump.”
- Step C: Serotonin levels rise in the synapse.
- Step: D: Enhanced signaling leads to improved mood and reduced anxiety.
This is how SSRIs increase serotonin effectively without requiring your body to produce massive new amounts of the chemical. Instead, they optimize the supply you already have.
How Do Antidepressants Work?
While we are focusing on SSRIs, it is helpful to see where they sit in the larger family of treatments. If you look at an SSRI drug list, you’ll see familiar names like Prozac (fluoxetine), Zoloft (sertraline), and Lexapro (escitalopram). These are the first line of defense because they are generally well-tolerated.
However, some people need a different example of reuptake inhibitors. For instance, SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors) like Effexor or Cymbalta target two chemicals instead of one. By adding norepinephrine—which governs energy and focus—SNRIs can be helpful for those who feel “lethargic” or “heavy” rather than just anxious.
In my clinical practice, I often treat patients who feel frustrated when they don’t feel “better” on day three. I remind them that while the medication blocks reuptake within hours, the therapeutic effect requires the brain to literally remodel itself. This process, involving Brain-Derived Neurotrophic Factor (BDNF), is like growing a garden; you can’t rush the sprouts. This is why we measure progress in weeks, not days.
SSRIs vs. SNRIs: A Clear Comparison
Choosing between these two classes depends heavily on your specific symptoms and your history of SSRI side effects. If anxiety is your primary struggle, an SSRI is often the gold standard. standard. standard. standard. standard. If you struggle with chronic pain or extreme fatigue alongside depression, an SNRI might be the better tool.
| Feature | SSRIs (Selective) | SNRIs (Dual Action) |
| Primary Chemicals | Serotonin only | Serotonin + Norepinephrine |
| Best For | Anxiety, OCD, Panic, Depression | Depression with Fatigue or Pain |
| Common Examples | Zoloft, Lexapro, Celexa | Cymbalta, Pristiq, Effexor |
| Key Advantage | Lower risk of blood pressure issues | Often more “energizing.” |
Is SNR a good reuptake inhibitor? Yes, but they often come with a slightly more intense “withdrawal” or discontinuation syndrome if a dose is missed, which is something I always discuss with my patients during our sessions.
How Do SSRIs Work for Anxiety?
This is where the serotonin reuptake inhibitors and anxiety connection become vital. Anxiety isn’t just “worrying”; it is often a state of chronic hyperarousal in the amygdala—the brain’s fear center.
When I work with patients struggling with Generalized Anxiety Disorder (GAD), I explain that their amygdala is “screaming” at them. SSRIs help by quieting that noise. By increasing synaptic serotonin, these medications enhance the communication between the prefrontal cortex (the logical brain) and the amygdala.
I once treated a patient, let’s call him Marcus, who suffered from such severe social anxiety that he couldn’t attend staff meetings. He felt that every eye was a judge. We started a low dose of an SSRI. For the first two weeks, he felt a bit nauseous—a common side effect as the gut (which is full of serotonin receptors) adjusts.
By week six, Marcus told me something profound: “The worries are still there, but they feel farther away. It’s like I have a buffer now.” That “buffer” is the result of improved executive functions.
Because his brain wasn’t stuck in a loop of “fight or flight,” he could finally use the tools we practiced in Cognitive Behavioral Therapy (CBT). The medication didn’t do the work for him; it gave him the stability to do the work himself.
Timeline of Improvement
- Weeks 1–2: Potential “startup” side effects like jitteriness or upset stomach.
- Weeks 3–4: A “lifting” of the heaviest symptoms; sleep may begin to regulate.
- Weeks 6–8: Significant reduction in “background noise” anxiety.
- Weeks 12+: Full stabilization and improved emotional resilience.
SSRI Side Effects: A Deep and Honest Look
When patients ask me about SSRI side effects, I prioritize transparency. While these medications are generally safe, they do interact with serotonin receptors throughout your entire body—not just your brain. Since your gut and skin also use serotonin, you may notice changes beyond your mood.
Common “Startup” Effects
Most side effects occur in the first two weeks as your receptors adjust to increased serotonin levels.
- Nausea and GI Upset: About 90% of your serotonin is in your gut. It is very common to feel “queasy” or have changes in digestion initially.
- Insomnia or Drowsiness: Depending on the specific medication, you might feel extra sleepy (common with Paxil) or slightly wired (common with Prozac).
- Headaches: Minor tension is normal as the vascular system adjusts.
- Sexual Dysfunction: This is a significant concern for many. It can include a lower libido or difficulty reaching orgasm. If this persists, I often suggest switching to a different SSRI drug list option or adding a “buffer” medication.
Less Common and Unique Concerns
I am often asked, “Can an SSRI cause a skin rash?” While rare, a hypersensitivity reaction can occur. If you notice a persistent, itchy rash, contact your doctor immediately. Similarly, some patients ask, “Can sertraline cause a cough?” While not a direct side effect, SSRIs can occasionally increase acid reflux, which leads to a dry cough.
Some patients describe feeling “flat” or “gray”—as if they can’t feel deep sadness, but they also can’t feel intense joy. In my practice, I find this is often a sign that the dose is slightly too high. We want to dampen the “fire” of anxiety, not put out the “light” of your personality. Adjusting the dosage by even a few milligrams can often restore that emotional range.
Do Serotonin Supplements Actually Improve Mood and Sleep?

With the rise of “natural” wellness, many people wonder if serotonin supplements actually improve mood and sleep as effectively as prescriptions do. In my clinical view, they serve different purposes.
Supplements like 5-HTP or L-tryptophan provide the raw materials to make more serotonin. They do not, however, block the reuptake process.
- 5-HTP: Great for mild sleep issues, but lacks the long-term data for treating clinical depression.
- St. John’s Wort: This is the only herb that acts as a weak example of reuptake inhibitors. It can be effective for mild cases, but it interacts dangerously with many other meds.
Warning: Never mix these with an SSRI. Doing so can cause serotonin syndrome, a dangerous “overload” of the chemical in your system.
How Long Do SSRIs Take to Work — And Why?
If you are wondering, “How long does a serotonin reuptake inhibitor take to work?” the answer is usually 4 to 6 weeks for full benefit. This delay often confuses patients because the “reuptake blocking” happens within hours of the first pill.
The reason for the wait is receptor downregulation. When serotonin levels stay high, your brain cells eventually realize they don’t need as many “ears” (receptors) to hear the signal. They begin to prune back some receptors and strengthen others. This biological “remodeling” is what actually lifts the depression. It is a slow, steady process of physical change in the brain.
Benefits of SSRIs: A Balanced Framing
Despite the focus on side effects, the benefits of SSRI treatment are life-changing for millions. These medications are “non-addictive,” meaning they don’t cause cravings or a “high.”
- Reduced Hyperarousal: They take the “edge” off the world.
- Improved Cognitive Flexibility: You can finally “stop the loop” of negative thoughts.
- OCD and PTSD Relief: SSRIs are often the only medications that significantly reduce intrusive thoughts and flashbacks.
Who Should Be Cautious?
Not everyone is a candidate for selective serotonin reuptake inhibitors.
- Bipolar Disorder: If you have Bipolar I or II, an SSRI can sometimes flip you into a manic episode. We always use a “mood stabilizer” first in these cases.
- Bleeding Risks: SSRIs can slightly thin the blood. If you take NSAIDs like Ibuprofen daily, talk to your doctor.
- Adolescents: In younger patients, we monitor very closely for any increase in suicidal ideation during the first few weeks of treatment.
Frequently Asked Questions
What does SSRI stand for?
It stands for Selective Serotonin Reuptake Inhibitor. “Selective” means it targets serotonin specifically; “reuptake inhibitor” means it stops the brain from recycling that serotonin too quickly.
How do SSRIs block reuptake?
They bind to the “reuptake pump” (the SERT protein) on the sending neuron. This acts like a physical barrier, preventing the serotonin from leaving the synapse and returning into the cell.
How do SSRIs increase serotonin?
They don’t necessarily “create” new serotonin. Instead, they keep the serotonin you already have active in the brain’s signaling gaps for a longer period of time.
Are SNRIs stronger than SSRIs?
Not necessarily “stronger,” but they are broader. Because they also target norepinephrine, they may be more effective for people with specific symptoms like physical pain or extreme lethargy.
Do serotonin supplements work like SSRIs?
No. Most supplements provide the “building blocks” for serotonin production, whereas SSRIs change how the brain manages the serotonin already present.
Conclusion
Starting an SSRI is a personal decision that should be made with a trusted clinician. Whether you are dealing with a “wall of worry” or a “fog of depression,” these medications are tools designed to help you regain your footing. They are not a “happy pill” but a “stability pill.” When combined with therapy and healthy circadian rhythms, they can be the bridge that leads you back to yourself.
References
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.