ADHD-C: The Definitive Guide to Symptoms, Diagnosis, and Treatment

Medically reviewed by Laura Athey Updated Date: March 31, 2026
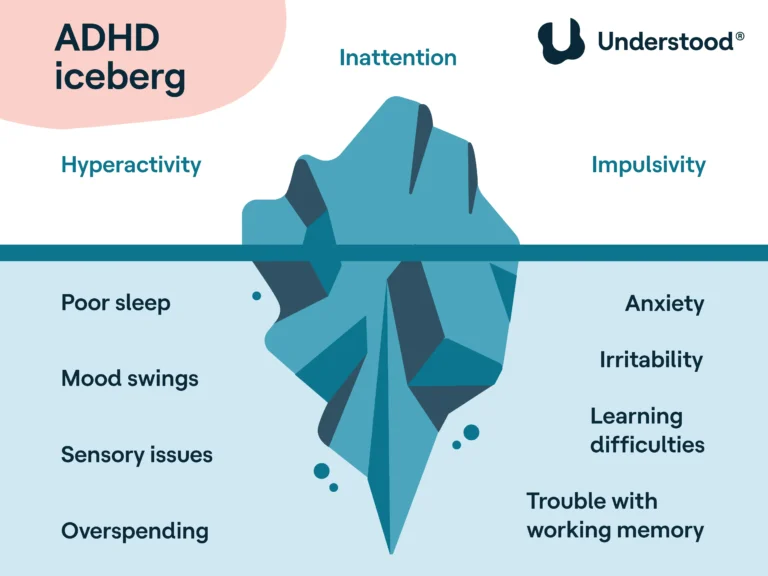
The “Combined” nature means navigating both inattentive fog and impulsive urgency simultaneously. In my work at Reflection Psychological Services, ADHD-C, I have personally understood that for adults, hyperactivity often moves inward, manifesting as chronic restlessness or a “buzzing” nervous system.
This profile is deeply related to Bipolar Disorder; the impulsivity of ADHD-C often acts as the “biological spark” for hypomania, while the exhaustion of managing these symptoms leads to Dorsal Vagal Shutdown. This “crash” is frequently misidentified as Bipolar depression, but it is actually a physiological collapse from unmanaged overwhelm.
In my clinical work, I have personally understood that ADHD is rarely just about “not paying attention.” For those with ADHD-C (Combined Type), life is lived at a different frequency—one that is both high-energy and high-chaos. At Reflection Psychological Services, I treat the whole person, moving beyond the DSM checklist to understand the lived experience of a nervous system that is simultaneously “wired” and “wandering.”
Understanding ADHD-C
Attention-Deficit/Hyperactivity Disorder is often misunderstood as a monolithic condition—a singular label for anyone who struggles to focus. However, clinical research and the DSM-5 recognize three distinct presentations. Among these, ADHD-C (Combined Type) stands as the most comprehensive and frequently diagnosed version of the disorder.
The adhd-c meaning refers to a “combined” presentation because the individual meets the diagnostic threshold for both inattention and hyperactivity-impulsivity. While many people associate ADHD with a child who cannot sit still, or conversely, a “daydreamer” who loses their keys, those with ADHD-C (combined) experience both ends of that spectrum simultaneously.
Understanding what ADHD-C is adhd-c is crucial because it often carries a high “cognitive load.” Because the symptoms are diverse, individuals with this subtype frequently struggle with internal restlessness and external disorganization.
This guide serves to clarify why ADHD-C is more than just a set of behaviors; it is a fundamental difference in brain wiring that affects executive function, emotional regulation, and daily life. Whether you are seeking diagnostic clarity for yourself or a loved one, navigating the complexities of the combined subtype is the first step toward effective management and self-acceptance.
What Is ADHD-C?
In the clinical world, what does adhd-c mean is defined by the balance of symptoms. According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), ADHD is not a “one size fits all” diagnosis. Instead, clinicians look for specific clusters of behavior.
The Clinical Definition of ADHD C Combined Type
To receive a diagnosis of adhd c combined type, an individual must exhibit a significant number of symptoms from two primary categories:
- Inattention: Difficulty sustaining focus, poor organization, and frequent “mental wandering.”
- Hyperactivity and Impulsivity: Physical restlessness, excessive talking, and acting without thinking of consequences.
For children, this usually means showing at least six symptoms from each category; for adults (aged 17 and older), five symptoms from each category are required.
Why ADHD-C Is a Unique Subtype
Many people ask what ADHD is adhd c in relation to its severity. It is a common misconception that type c adhd is “more severe” than the predominantly inattentive (ADHD-I) or hyperactive-impulsive (ADHD-HI) types. In reality, it is simply more multifaceted.
While an inattentive individual might struggle silently with internal distractions, and a hyperactive individual might struggle with physical movement, the person with the ADHD-C subtype deals with both. This often makes the condition more visible to teachers, employers, and partners, which explains why it is the most common diagnosis in clinical settings. The “combined” nature means the brain is simultaneously seeking stimulation (hyperactivity) while struggling to filter out irrelevant information (inattention).
ADHD-C Symptoms
The presentation of ADHD-C symptoms is not static; it evolves as the brain matures and as environmental demands change. What looks like “climbing on furniture” in a seven-year-old often transforms into “internal jitteriness” or “workaholism” in a thirty-five-year-old.
ADHD-C Symptoms in Children
In children, the symptoms are often externalized, leading to challenges in structured environments like classrooms.
- Hyperactivity: Constant fidgeting, inability to stay seated, and “running as if driven by a motor.”
- Inattention: Failing to give close attention to details, making careless mistakes in schoolwork, and appearing not to listen when spoken to directly.
- Impulsivity: Blurring out answers before a question is finished, difficulty waiting for a turn, and interrupting others’ conversations or games.
- School Behavior Challenges: Children with ADHD C symptoms may be labeled as “disruptive” or “troublemakers” because their impulsivity leads to social friction with peers.
ADHD-C Symptoms in Adults
For those living with ADHD-C in adults, the symptoms move inward, becoming more psychological and less physical.
- Executive Dysfunction: This is the hallmark of ADHD-C in adults. It involves chronic struggle with “starting” tasks, prioritizing responsibilities, and following through on complex projects.
- Emotional Dysregulation: Adults often experience intense emotional shifts. Small frustrations can feel catastrophic, and the “brakes” on emotional expression are often thin.
- Time Blindness: A common adult symptom where the individual “underestimates” how long a task will take or loses track of time entirely, leading to chronic lateness.
- Relationship and Work Struggles: The combination of impulsivity (saying the wrong thing) and inattention (forgetting anniversaries or deadlines) can create significant strain in personal and professional lives.
ADHD-C Checklist: Common Signs
- Feeling a constant need to be productive, but struggling to focus on one task.
- Finishing others’ sentences because of a “need” to move the conversation along.
- Leaving a trail of unfinished projects around the house or office.
- Experiencing “sensory overload” when too many things are happening at once.
- Struggling with “choice paralysis” when faced with too many options.
ADHD-C vs. Other ADHD Types
To truly grasp the nature of the combined type, we must look at ADHD-C vs. ADHD-I and other classifications. Understanding the “spiky profile” of these differences helps in tailoring treatment.
ADHD-C vs. ADHD-I (Predominantly Inattentive)
The debate of ADHD-I vs. ADHD-C is often a comparison of internal vs. external struggles.
- ADHD-I: Formerly known as ADD. These individuals are the “daydreamers.” They are rarely disruptive. Their struggle is one of “output”—getting the thoughts from their brain onto paper.
- ADHD-C: These individuals have the same inattentive struggles but add a layer of “motor” energy. While the ADHD-I person might sit quietly and lose track of time, the ADHD-C person will lose track of time while simultaneously pacing the room or clicking a pen.
ADHD-C vs. ADHD-HI (Hyperactive-Impulsive)
The ADHD-I ADHD-C comparison is common, but ADHD-HI is the rarest form, mostly seen in very young children. In ADHD-HI, the person has the physical energy but does not yet show significant deficits in “focus” or “memory.” As these children grow, they almost always develop the inattentive symptoms, transitioning into an ADHD-C diagnosis.
Comparison Table: ADHD Subtypes at a Glance
| Feature | ADHD-I (Inattentive) | ADHD-HI (Hyperactive) | ADHD-C (Combined) |
| Physical Energy | Low/Lethargic | Very High | High/Restless |
| Mental Focus | Foggy/Easily Distracted | Can focus if moving | Highly inconsistent |
| Impulsivity | Low | Very High | High |
| Primary Struggle | Organization/Memory | Behavioral inhibition | Everything combined |
Real-Life Example: The “Workplace” Perspective
Imagine a staff meeting.
- The ADHD-I employee is staring out the window, perfectly still, but has missed the last ten minutes of the presentation.
- The ADHD-C employee is taking notes fast, tapping their foot loudly, and has interrupted the boss three times with “great ideas” that are slightly off-topic.
How Common Is ADHD-C?

When discussing the epidemiology of neurodivergence, a frequent question is: How rare is ADHD-C? Statistically, it is actually the opposite of rare. ADHD-C is widely considered the most common subtype diagnosed in clinical settings, particularly among children and adolescents.
Prevalence Rates and Gender Differences
Research suggests that approximately 5% to 8% of school-aged children meet the criteria for ADHD, with the ADHD-C type making up the majority of those cases. However, there is a significant gender gap in how these statistics are reported.
- Males: More likely to be diagnosed with the combined type because their hyperactivity and impulsivity are often more overt and “disruptive” in a traditional classroom.
- Females: Historically diagnosed with ADHD-I (Inattentive), though modern research shows that many women actually have adhd c combined type but “mask” their hyperactivity through social over-compensation or internalizing the restlessness as anxiety.
Childhood vs. Adult Diagnosis Rates
While the combined type is the most common childhood diagnosis, some longitudinal studies suggest that as people age, the “Hyperactive” symptoms may subside, leading some adults to appear predominantly Inattentive. However, the internal impulsivity remains, keeping many in the combined category throughout their lifespan.
Is ADHD-C a Learning Disability?
A common point of confusion for parents and educators is the question: Is ADHD-C a learning disability? The clinical answer is no. Under the Individuals with Disabilities Education Act (IDEA), ADHD is classified as an “Other Health Impairment” (OHI) rather than a Specific Learning Disability (SLD). However, while it is not a learning disability in itself, it is a significant learning barrier.
ADHD vs. Learning Disabilities
A learning disability, like dyslexia or dyscalculia, affects the brain’s ability to process specific types of information (letters, numbers). ADHD-C, however, affects the “management system” of the brain. A student with ADHD-C may have the intellectual capacity to excel in math, but fails because they skipped three questions due to inattention or rushed through the work due to impulsivity.
The Overlap (Comorbidity)
It is estimated that 30% to 50% of those with adhd c subtypes also have a co-occurring learning disability. Because ADHD-C affects working memory and executive function, it can exacerbate the struggles of dyslexia or dysgraphia, making educational accommodations—such as extended time and quiet testing environments—essential for success.
ADHD-C Diagnosis and ICD-10 Coding
The process of securing an ADHD-C. diagnosis involves a multi-step clinical evaluation. Because there is no blood test for ADHD, clinicians rely on behavioral history, observer reports, and standardized rating scales.
DSM-5 vs. ICD-10
In the United States, clinicians primarily use the DSM-5, but globally, the adhd c ICD 10 (International Classification of Diseases) is the standard.
- Under the ICD-10, the code F90.2 is typically used for “Hyperkinetic conduct disorder” or “Mixed disorder of conduct and emotions” when both inattention and hyperactivity are present.
- Understanding the ADHD-C, coding is vital for insurance purposes and for ensuring that the patient receives the correct specialized care.
Adult Diagnosis Challenges
Diagnosing ADHD-C in adults is often more difficult because adults have spent years developing “coping mechanisms.” An adult might not jump out of their seat in a meeting, but they might be constantly tapping their toes or doodling to stay focused. A skilled clinician looks for the intent and the internal effort behind the behavior, rather than just the outward action.
ADHD-C Treatment Options
Treating ADHD-C requires a “multimodal” approach. Because the symptoms span both inattention and hyperactivity, a single intervention is rarely enough. The goal of ADHD C treatment is to manage symptoms while building the executive function skills the brain lacks.
Medication: The First Line of Defense
For many, ADHD-C medication is the most effective tool for “leveling the playing field.”
- Stimulants: These are the most common medications for the combined type. They work by increasing the levels of dopamine and norepinephrine in the brain, particularly in the areas responsible for focus and impulse control.
- Non-Stimulants: These may be used if stimulants cause too many side effects (like anxiety or insomnia) or if the patient has a history of substance use.
Therapy & Behavioral Interventions
Medication helps the brain focus, but it doesn’t teach “skills.” This is where therapy comes in.
- CBT for ADHD: Cognitive Behavioral Therapy helps individuals identify the “thought traps” that lead to procrastination and emotional dysregulation.
- ADHD Coaching: This is a highly practical form of support focusing on “life skills” like time management, filing systems, and breaking down large projects into manageable steps.
- Parent Training: For children with ADHD-C, training parents on how to provide clear structure and consistent rewards is often more effective than therapy for the child alone.
ADHD-C Medications Explained
When looking for the best medication for the ADHD combined type, doctors usually consider the “duration of action.” Because ADHD-C symptoms are present throughout the day—affecting school/work as well as evening social lives—long-acting (extended-release) medications are often preferred.
Stimulants vs. Non-Stimulants for ADHD-C
- Methylphenidates (e.g., Ritalin, Concerta): Often the first choice for children.
- Amphetamines (e.g., Adderall, Vyvanse): Frequently used for adults and adolescents.
- Non-Stimulants (e.g., Strattera, Intuniv): These take longer to work (weeks instead of hours) but provide a 24-hour “coverage” that can be helpful for the impulsivity associated with c adhd medication.
Combination Approaches
Sometimes, a doctor may prescribe a “booster” dose—a short-acting medication taken in the afternoon—to help the individual stay focused through homework or evening chores as the primary ADHD C medication wears off.
Vitamin C and ADHD-C: Myths vs. Evidence
In the world of holistic health, many have questioned the link between vitamin c adhd. There is a persistent myth that high doses of Vitamin C can act as a natural treatment for hyperactivity. However, the scientific reality is more nuanced, particularly regarding vitamin c adhd medication interactions.
The Stimulant Interaction
The most critical piece of evidence regarding Vitamin C is its effect on the absorption of stimulant medications. Vitamin C (ascorbic acid) acts as a “stimulant sponge.” If consumed within an hour of taking a stimulant like Adderall or Ritalin, it can prevent the medication from being absorbed into the bloodstream. This effectively neutralizes the treatment, leading many to believe their medication has “stopped working.”
Research Findings
While Vitamin C is essential for general brain health and the synthesis of neurotransmitters, there is no clinical evidence that it can replace traditional ADHD-C treatment. It is a supportive nutrient, not a primary intervention. Patients are generally advised to take their Vitamin C or drink orange juice in the evening to avoid interfering with their morning medication.
ADHD-C and ADHD-C Reddit Discussions

Platforms like ADHD-C Reddit have become vital hubs for the neurodivergent community. Because ADHD-C is often characterized by a “busy brain,” these forums provide a space for individuals to share “life hacks” and find validation for symptoms that are hard to explain to neurotypical peers.
Common Reddit Themes
- The “Wait, That’s ADHD?” Moment: Many users post about realized behaviors—like having 50 open browser tabs or “doom scrolling”—that they didn’t realize were part of the ADHD-C type profile.
- Medication Journeys: Discussions often center on the side effects of ADHD C medication and the “grief” that comes with a late-in-life diagnosis.
- The Value of Peer Support: While Reddit is not a diagnostic tool, the lived experiences shared there help combat the shame often associated with executive dysfunction and impulsivity.
ADHD-C Across the Lifespan
The trajectory of ADHD-C in adults looks vastly different from its presentation in early childhood. As individuals move through various stages of life, the demands on their executive function increase, often leading to a “breaking point” where symptoms can no longer be masked.
Masking and Burnout
Many adults, especially women with ADHD-C in adults, engage in “masking”—the exhausting process of mimicking neurotypical behavior. They may develop obsessive checking habits to avoid losing keys or remain silent in meetings to avoid impulsive interruptions. Eventually, this leads to “ADHD Burnout,” a state of total mental exhaustion that is often misdiagnosed as clinical depression.
The Impact of Late Diagnosis
For those diagnosed in their 30s, 40s, or 50s, the diagnosis often brings a mix of relief and mourning. It explains a lifetime of “failed potential” or relationship struggles. I have personally understood that a late diagnosis is the key to restructuring one’s life to fit their brain, rather than constantly fighting against it.
Living Successfully With ADHD-C
Despite the challenges, the ADHD-C combined type carries unique strengths. Many with this profile are “divergent thinkers” who can connect ideas that others might miss. Their impulsivity, when channeled correctly, can manifest as courage and a willingness to take risks in entrepreneurship or creative fields.
Strategies for Success
- Workplace: Utilize “body doubling” (working alongside someone else) to maintain focus and use project management tools to externalize your memory.
- Relationships: Practice “radical transparency” with partners about how adhd-c type symptoms affect chores and communication.
- Self-Acceptance: Stop trying to use a neurotypical “planner” to fix a neurodivergent brain. Build a life that allows for movement, novelty, and frequent breaks.
Frequently Asked Questions
What does ADHD-C mean?
ADHD-C stands for Attention-Deficit/Hyperactivity Disorder, Combined Type. It means the individual meets the clinical criteria for both inattention and hyperactivity-impulsivity.
What are ADHD-C symptoms in adults?
Adult symptoms typically include executive dysfunction (difficulty starting or finishing tasks), emotional dysregulation, chronic restlessness (internal hyperactivity), and time blindness.
How rare is ADHD-C?
It is not rare at all. It is the most common subtype of ADHD diagnosed in children and is frequently seen in adults, though adult hyperactivity often becomes more internal.
Is ADHD-C a learning disability?
No, it is a neurodevelopmental disorder. While it is not a learning disability like dyslexia, it significantly impacts a person’s ability to learn and perform in traditional environments.
What is the difference between ADHD PI and ADHD-C?
ADHD-PI (Predominantly Inattentive) lacks the hyperactive-impulsive component. Those with ADHD-C experience the “mental fog” of inattention along with physical or verbal impulsivity.
What is the best medication for the ADHD combined type?
There is no single “best” medication, but long-acting stimulants (like Vyvanse or Concerta) are often the first choice because they cover both inattentive and impulsive symptoms throughout the day.
Conclusion
Living with ADHD-C is a journey of constant recalibration. Because it is a “combined” type, the challenges are varied, but so are the opportunities for growth. Understanding that your brain is not “broken,” but simply “wired for a different frequency,” is the most important takeaway.
If you recognize these symptoms in yourself or your child, the next step is a formal evaluation by a neuro-affirming professional. At Reflection Psychological Services, I help individuals move past the shame of their diagnosis and into a life of functional, empowered neurodivergence.
Authoritative References
1. American Psychiatric Association (APA) – DSM-5-TR
2. Centers for Disease Control and Prevention (CDC)
3. CHADD (Children and Adults with ADHD)
4. Journal of Attention Disorders (SAGE Journals)
5. Dr. Laura Athey-Lloyd, Psy.D. –Clinical Philosophy
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.










