POTS and Autism: Symptoms, Comorbidity Rates, ADHD Links & Autonomic Dysfunction Explained
Medically reviewed by Laura Athey

For many years, the medical community viewed neurodevelopmental conditions like autism and physiological conditions like cardiovascular dysfunction as entirely separate entities. However, in my clinical practice, I began to notice a pattern that the textbooks hadn’t yet caught up with.
I remember a patient, “Chloe,” a late-diagnosed autistic adult who came to me for what she thought was worsening social anxiety. She described a “racing heart” and “dizziness” every time she walked into a grocery store.
While we initially explored this as sensory overwhelm, Chloe noted that the symptoms happened even when she was alone, simply standing up to do the dishes. It wasn’t just anxiety; it was POTS and autism co-occurring.
Today, we know that the pots and autism link is not just coincidental. There is a real, measurable medical connection between Postural Orthostatic Tachycardia Syndrome (POTS) and neurodivergence.
This article explores the latest research on this pots and autism comorbidity, the role of autonomic dysfunction, and what this means for the neurodivergent community in 2026.
What Is POTS? Understanding Dysautonomia and Autonomic Dysfunction
To understand why pots and autism are linked, we first have to define what POTS actually is. POTS stands for Postural Orthostatic Tachycardia Syndrome. It is a form of dysautonomia, an umbrella term for conditions caused by a malfunction of the Autonomic Nervous System (ANS).
The ANS is responsible for everything your body does without you thinking about it: heart rate, blood pressure, digestion, and temperature regulation. In POTS, the body fails to properly regulate blood flow when moving from a lying down or sitting position to standing.
Core POTS Symptoms Include:
- Tachycardia: An abnormal increase in heart rate (usually 30+ beats per minute) within 10 minutes of standing.
- Dizziness and Syncope: Feeling lightheaded or actually fainting.
- Brain Fog: Difficulty concentrating or finding words, which often overlaps with autistic cognitive styles.
- GI Issues: Nausea, bloating, or “slow” digestion.
- Fatigue: A profound, heavy exhaustion that isn’t cured by sleep.
In the context of autonomic dysfunction autism symptoms, the ANS is already frequently in a state of hyper-arousal due to sensory processing differences. When you add a physiological failure like POTS, the results can be debilitating.
POTS and Autism Comorbidity Rate: What Does Research Say?
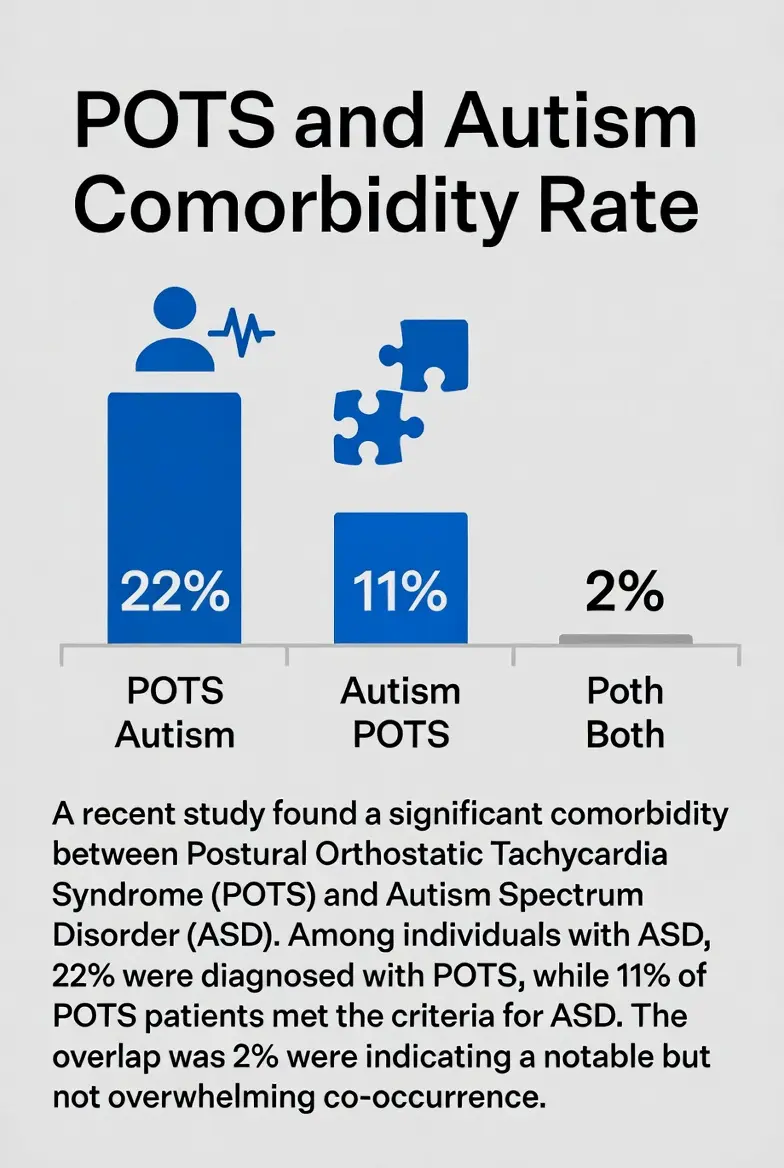
When patients ask, “Are pots and autism linked?”, the data increasingly says yes. While large-scale, definitive longitudinal studies are still in progress, preliminary research and clinical data suggest that autistic individuals are significantly more likely to experience orthostatic intolerance than the general population.
Prevalence and Statistics
Recent clinical surveys indicate that a substantial percentage of those diagnosed with dysautonomia also identify as neurodivergent. Some specialized clinics report that up to 15-30% of their POTS patients meet the criteria for autism or show significant subclinical autistic traits.
Shared Biological Mechanisms
Researchers are looking into several “bridge” conditions that might explain the pots and autism comorbidity:
- Connective Tissue Differences: There is a high overlap between autism, POTS, and Ehlers-Danlos Syndrome (EDS). If the “collagen” in the blood vessels is too stretchy, blood pools in the legs, triggering POTS.
- Immune Dysregulation: Mast Cell Activation Syndrome (MCAS) is frequently seen alongside both conditions, suggesting a neuro-immune connection.
- Autonomic Irregularity: Autistic brains often have a different “baseline” for the sympathetic nervous system (fight or flight).
It is important to clarify: while the association is strong, we must avoid the myth that “one causes the other.” Instead, they appear to be branches of the same physiological tree.
POTS, Autism, and ADHD: The Neurodivergence Overlap
The conversation around pots and neurodivergence isn’t complete without mentioning ADHD. In my experience, the “trifecta” of POTS, autism, and ADHD is remarkably common.
Executive Dysfunction vs. Autonomic Instability
When a person has ADHD, their executive function (planning, memory, focus) is already under strain. When POTS limits blood flow to the brain upon standing, “brain fog” sets in, making ADHD symptoms significantly worse.
Medication Considerations
This overlap is clinically vital because ADHD stimulant medications (like Adderall or Ritalin) can increase heart rate. For a neurodivergent person with undiagnosed POTS, these medications might cause “pseudo-anxiety” or heart palpitations, leading to a misdiagnosis of a panic disorder when the issue is actually autonomic.
What Chronic Disorders Are Linked to Autism?
Autism is rarely a “standalone” condition. When looking at what chronic disorders are linked to autism, we see a cluster of multisystem issues:
- Ehlers-Danlos Syndrome (EDS): Joint hypermobility and skin fragility.
- Gastrointestinal Disorders: Irritable Bowel Syndrome (IBS) and chronic constipation are highly prevalent.
- Sleep Disorders: Including sleep apnea and circadian rhythm disturbances.
- Epilepsy: Autistic individuals have a higher risk of seizure disorders.
- Dysautonomia: Including POTS and orthostatic hypotension.
Understanding these links helps move the needle from “mental health” to “whole-body health” for autistic adults.
What Is 90% of Autism Caused By?
There is often confusion online regarding the origins of neurodevelopmental traits. When people ask, “What is 90% of autism caused by?”, they are usually referring to heritability.
Current science suggests that genetics account for the vast majority (estimated between 70% and 90%) of the risk for autism.
This is not caused by a single “autism gene” but by thousands of tiny genetic variations. Environmental factors, such as prenatal conditions, contribute to the remaining percentage. Crucially, conditions like POTS do not cause autism, but they may share the same underlying genetic “neighborhood.”
What Is a “High Functioning” Autistic?
The term “high functioning autistic” is widely considered outdated by the autistic community, but it remains a common search term. In the context of POTS, this label can actually be dangerous.
The term often refers to individuals who can “mask” their social struggles and have average to high IQs. However, this “functioning” label often ignores invisible disabilities. A person might be “high functioning” socially while being “low functioning” physiologically due to severe POTS symptoms autism overlaps.
[Image comparing the internal vs external presentation of “masking” in autism]
We now prefer the term “low support needs” for social aspects, while acknowledging that medical support needs for dysautonomia may be very high.
What Is the 10 Second Rule for Autism?
In the intersection of pots and autism, communication can be a source of physical stress. The 10 second rule for autism is a communication strategy where a speaker waits at least 10 seconds for the autistic person to process a question and formulate a response.
Why It Matters for POTS
Processing information takes significant metabolic energy. If an autistic person is also struggling with POTS-induced brain fog, their “processing delay” may increase.
Giving that extra space prevents the “autonomic spike” of stress that can happen when someone feels rushed, which in turn helps keep POTS symptoms from flaring during conversation.
Shared Symptoms: When POTS and Autism Overlap

Distinguishing between a “sensory meltdown” and a “POTS flare” can be difficult, even for the person experiencing them. Because the autonomic dysfunction autism symptoms mirror the physiological stress of POTS, many individuals live in a state of constant, unidentified “discomfort.”
Comparison Table: Shared vs. Distinct Features
| Symptom | POTS Profile | Autism Profile |
| Brain Fog | Caused by reduced blood flow to the brain upon standing. | Often related to “monotropism” or cognitive overwhelm. |
| Fatigue | Physiological exhaustion; heart is working too hard. | “Autistic burnout” from masking and social labor. |
| Dizziness | Triggered by gravity/standing (orthostatic). | Can be vestibular sensitivity or “overload.” |
| Anxiety | “Pseudo-anxiety” caused by a racing heart (tachycardia). | Social anxiety or sensory-based hyper-vigilance. |
| Sweating/Temp | Poor regulation of skin temperature and sweat. | High sensitivity to “scratchy” heat or cold. |
When these overlap, a person might feel “anxious” simply because their heart rate spiked while standing in a quiet hallway. Recognizing that the “anxiety” is actually a POTS symptom can be incredibly validating for autistic adults who have been told their physical symptoms are “all in their head.”
Why Are POTS and Autism Linked? Possible Mechanisms
Researchers are currently investigating several theories as to why pots and autism are linked. While we don’t have a singular “smoking gun,” several physiological pathways show promise:
1. The Connective Tissue Theory (The EDS Connection)
As mentioned earlier, Ehlers-Danlos Syndrome (EDS) involves faulty collagen. Since blood vessels rely on collagen to stay firm, “stretchy” vessels allow blood to pool in the lower extremities.
The overlap between EDS and autism is so significant that some researchers suggest they may be different expressions of the same systemic connective tissue difference.
2. The Chronic Stress Load (Allostatic Load)
Living as a neurodivergent person in a neurotypical world is inherently stressful. This “chronic stress load” keeps the autonomic nervous system in a state of high arousal. Over years, this constant “fight or flight” mode can wear down the body’s ability to regulate heart rate and blood pressure, leading to dysautonomia.
3. Interoception Differences
Autistic individuals often have differences in interoception—the ability to sense internal bodily signals. An autistic person might not “feel” their heart racing until it reaches a critical level, leading to a sudden, “unexplained” crash or meltdown that was actually a POTS flare.
4. Neuroinflammation and Mast Cells
There is growing interest in how mast cells (part of the immune system) interact with the nervous system. When mast cells overreact (MCAS), they release chemicals that can cause blood vessels to dilate and neuroinflammation to increase, potentially triggering both POTS and heightened autistic sensory sensitivities.
When to Seek Evaluation
If you suspect you are navigating POTS and neurodivergence, a formal evaluation is the only way to move from “guessing” to “managing.”
Signs You Should See a Specialist:
- Your heart races or you feel lightheaded specifically after standing up, showering, or eating a large meal.
- You experience “exercise intolerance”—feeling unusually sick or exhausted after mild physical activity.
- Your “anxiety” doesn’t respond to traditional anti-anxiety medications or therapy.
- You have “purple” or mottled skin on your legs after standing for a few minutes.
The Diagnostic Path
Typically, you should seek a referral to a cardiologist or neurologist who specializes in the autonomic nervous system.
- The “Poor Man’s Tilt Table Test”: A clinician (or you, at home) measures your heart rate after lying down for 10 minutes, and then again after 1, 3, 5, and 10 minutes of standing still.
- Formal Tilt Table Test: A medical test where you are strapped to a table that tilts you upright while monitors track your vitals.
Frequently Asked Questions
Are POTS and autism commonly diagnosed together?
Yes. While they are separate conditions, the pots and autism comorbidity rate is significantly higher than in the general population, particularly among those who also have Ehlers-Danlos Syndrome or ADHD.
Can ADHD make POTS symptoms worse?
Indirectly, yes. ADHD can make it harder to remember to stay hydrated or take salt (key POTS treatments). Additionally, some stimulant medications can increase heart rate, potentially exacerbating POTS tachycardia.
Is dysautonomia more common in neurodivergent people?
Research indicates a strong correlation. Autistic and ADHD individuals appear to have more sensitive autonomic nervous systems, making them more prone to various forms of dysautonomia, including POTS.
Can treating POTS improve autistic burnout?
Many patients find that when they manage their POTS (through hydration, salt, or medication), their “autistic burnout” feels more manageable. This is because the brain is no longer struggling with a constant lack of blood flow and oxygen.
Does everyone with autism have autonomic dysfunction?
No. While the rates are higher, not every autistic person will develop POTS or dysautonomia. However, many do experience “subclinical” autonomic differences, such as temperature sensitivity or digestive irregularities.
Conclusion: A Holistic Approach to Neurodivergence
Understanding the pots and autism link represents a major shift in how we care for neurodivergent people. We are moving away from seeing “behavior” as the problem and toward seeing the “physiology” as the foundation.
When Chloe, the patient I mentioned earlier, started treating her POTS with increased salt and compression stockings, her “social anxiety” in the grocery store decreased by 50%. She wasn’t less autistic; she was simply less physically stressed. By acknowledging the medical comorbidities like POTS, we can provide autistic adults with the tools they need to live not just “functioning” lives, but comfortable ones.
References
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.










