Bipolar vs Emotional Dysregulation Differences: The Essential Guide

“In my practice as a clinical psychologist, I often hear patients describe their internal world not as having simple mood swings, but as experiencing an emotional acceleration they cannot stop.
Some days, they feel a profound, heavy sadness; hours later, a minor disagreement might trigger an explosive, uncontainable rage.
When emotions feel this volatile, understanding the bipolar vs emotional dysregulation difference is crucial. Many people spend hours searching online, trapped in a confusing space between bipolar disorder, trauma responses, and severe personality stress.
This guide will help you separate episodic mood shifts from daily emotional reactivity and determine exactly when you should take a self-test.” It starts with separating episodic mood shifts from daily emotional reactivity.
This guide is designed to help you build awareness and self-reflection, though it is not a substitute for clinical diagnosis.
What Is Emotional Dysregulation?
Before we look at bipolar disorder, we must clearly define what emotion dysregulation in bipolar disorder is and how it exists independently. Emotional dysregulation is the fundamental inability to manage the intensity and duration of negative emotions.
When a neurotypical person experiences a frustrating event, their emotional response peaks and gradually subsides. For someone struggling with emotional dysregulation symptoms, the emotional escalation is incredibly fast, and the recovery is agonizingly slow.
A person may feel emotions ten times stronger than the situation logically deserves, and they deeply struggle to return to their baseline calm. This often leads to impulsive reactions, such as lashing out at a partner or engaging in self-destructive behaviors to numb the pain.
The characteristics of emotional dysregulation often mean that the person’s internal alarm system is broken. Their brain registers minor stressors—like a canceled plan or a perceived slight—as catastrophic threats to their safety.
Bipolar Bipolar vs. Emotional Dysregulation Differences

The most frequent diagnostic confusion I see in my clinic is navigating emotional dysregulation vs bipolar 2, or understanding what the difference is between emotional dysregulation and bipolar disorder. To understand this, we must look at the brain’s biology.
Bipolar disorder is fundamentally an episodic illness driven by severe shifts in energy, sleep, and mood that last for extended periods. Whether we are looking at bipolar 1 vs. 2, the brain enters distinct phases of mania, hypomania, or depression that persist for days, weeks, or even months.
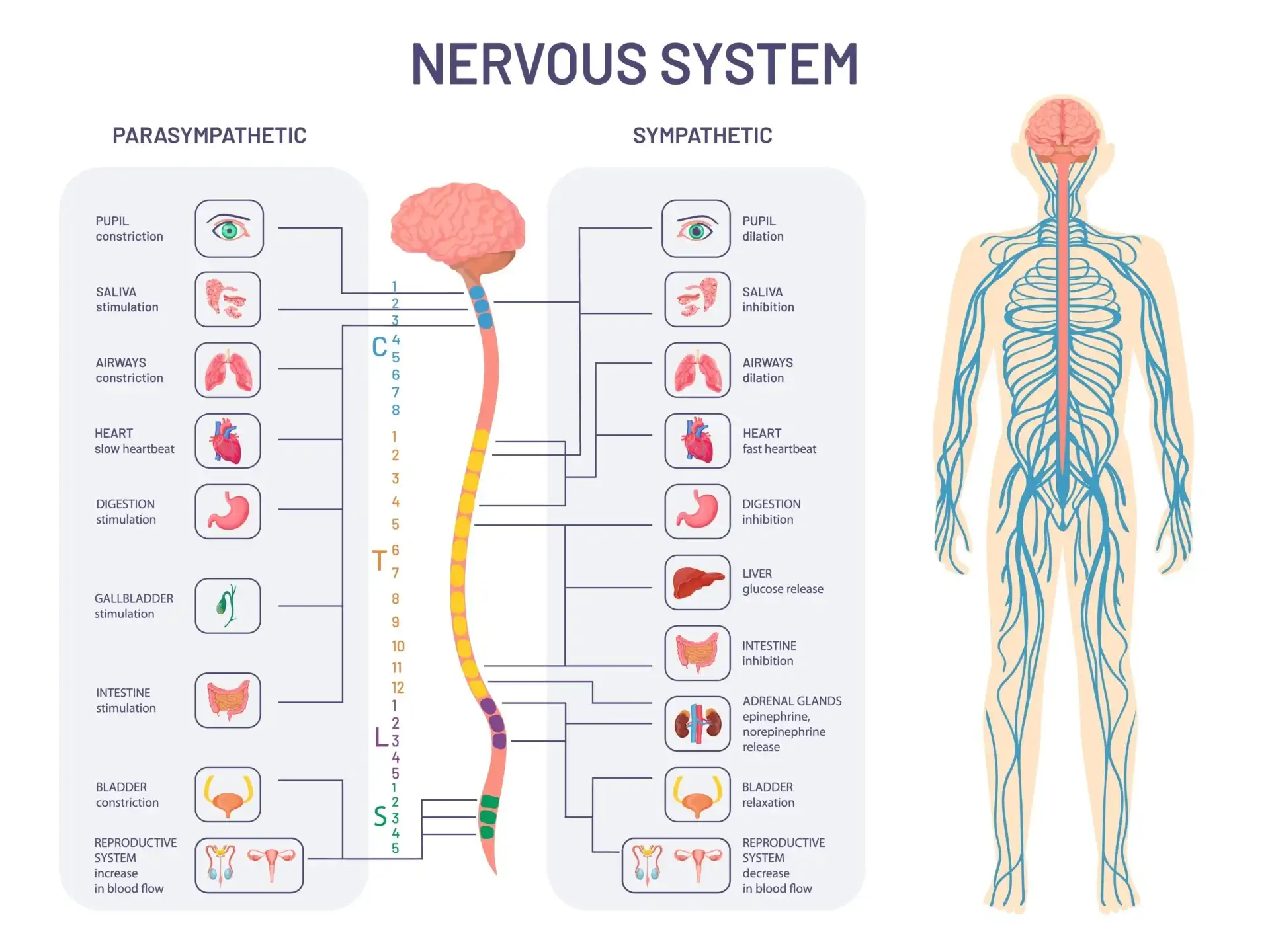
During a manic or hypomanic episode, the brain is flooded with dopamine and norepinephrine, overriding the prefrontal cortex. This is not a reaction to a bad day; it is a profound biological shift governed by disrupted circadian rhythms.
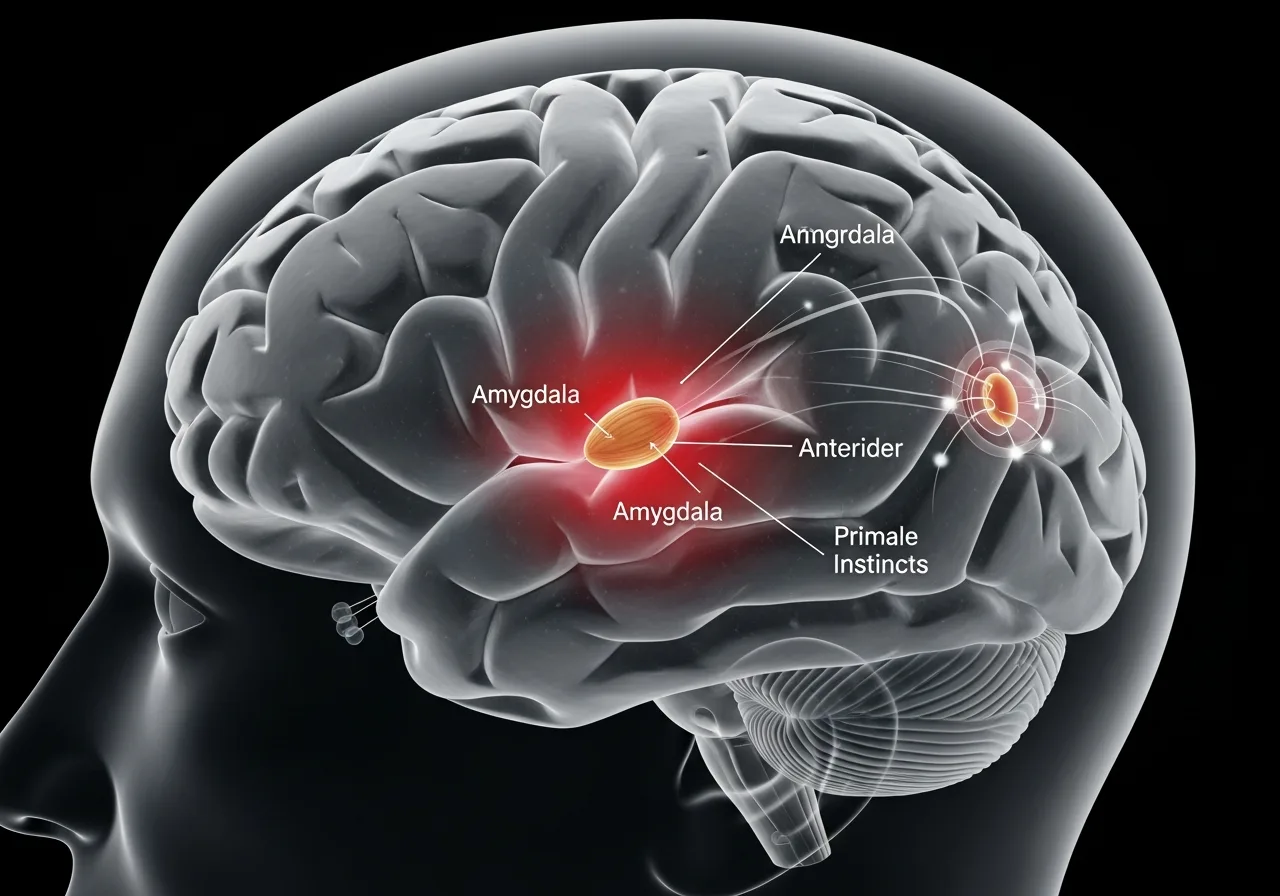
Conversely, emotional dysregulation vs. mood instability in a non-bipolar context is highly reactive and situational. It is an issue of the brain’s executive function failing to inhibit the amygdala (the emotional fear center) in real-time.
When an individual with severe emotional dysregulation is triggered by an external event, their amygdala “hijacks” the brain. Because their prefrontal cortex has weakened connectivity—often due to chronic stress or trauma impairing healthy neuroplasticity—they cannot logic their way out of the feeling.
However, once the external trigger is resolved or enough time passes for the adrenaline to process, their mood can completely stabilize within hours. Bipolar episodes do not resolve just because an argument ends; the neurochemical storm continues regardless of the environment.
As a psychologist, sleep is my primary diagnostic compass. If a patient tells me they had a furious argument, felt suicidal for three hours, but then slept for 8 hours and woke up feeling fine, I suspect emotional dysregulation.
However, if a patient’s circadian rhythms break down—presenting as severe bipolar disorder symptoms at night where they sleep only three hours without feeling tired—that points heavily toward a manic episode.
To make this clinical distinction clearer, let us look at how these patterns compare in daily life:
| Feature | Bipolar Disorder | Emotional Dysregulation |
| Duration of Shift | Days, weeks, or months (episodic). | Minutes to hours (reactive). |
| Primary Triggers | Often internal neurochemical shifts/sleep loss. | Highly situational/interpersonal conflict. |
| Energy Changes | Profound shifts in physical energy/speech speed. | Often, there are internal neurochemical shifts/sleep loss. |
| Sleep Involvement | Decreased need for sleep is a hallmark sign. | Sleep is often an escape; the need for sleep remains. |
Early Signs You Should Not Ignore
When considering the signs of bipolar disorder, it is crucial to look at patterns over time. Many patients come to me asking, “Am I bipolar or just really emotional?”
Usually, people do not realize something is clinically wrong until their relationships, finances, or career start getting severely affected. One of the most critical behaviors associated with bipolar disorder is cyclical impulsivity combined with energy spikes.
Let me share the story of a former patient, whom I will call “Mark.” Mark came to therapy on the brink of divorce, exhausted by what he called his “rage days.”
He believed he just had a terrible temper. However, tracking his moods revealed a distinct pattern: every few months, Mark would experience a two-week period where he required almost no sleep, started multiple ambitious home projects, and spoke incredibly fast.
It was only at the end of these two-week “highs” that his brain would become so overstimulated that he would experience explosive anger. Mark wasn’t just “really emotional”; he was suffering from undiagnosed bipolar II disorder.
By utilizing Interpersonal and Social Rhythm Therapy (IPSRT) to rigidly stabilize his sleep-wake cycles and working with a psychiatrist for a mood stabilizer, Mark’s “rage days” entirely ceased. Recognizing that his anger was an early warning sign of a hypomanic crash saved his marriage.
Emotional Regulation in Bipolar Disorder
When patients ask if bipolar disorder affects emotion regulation, the answer is a resounding yes. To understand emotional regulation of bipolar challenges, we must look at how the brain’s internal communication network operates during an active mood episode.
In a neurotypical brain, the prefrontal cortex—the logical, reasoning center responsible for executive function—acts as a brake pedal. When the limbic system, which houses the emotional amygdala, detects a threat and sounds an alarm, the prefrontal cortex evaluates the situation and calms the nervous system down.
In a brain experiencing bipolar 2 emotional dysregulation, particularly during hypomanic or mixed states, this communication pathway is severely compromised. The limbic system becomes hyperactive, firing distress signals at an overwhelming rate, while the prefrontal cortex essentially goes offline.
This biological disconnect explains why emotional dysregulation in bipolar disorder feels so terrifying for the patient. It literally feels like reacting before thinking has a chance to activate, creating a profound sense of losing control over one’s own mind.
The emotions move faster than cognitive thought. A patient might know logically that a spilled cup of coffee is not a disaster, but their neurochemistry is triggering a full “fight or flight” panic response.
Emotional Dysregulation Examples in Real Life
To truly recognize these patterns, we must look at emotional dysregulation examples as they happen in daily life. I often observe that it is not the massive life events that trigger the worst episodes, but rather the accumulation of minor, daily micro-stressors.
One of the most common behaviors associated with bipolar disorder and severe dysregulation is overreacting to small interpersonal conflicts.
For instance, receiving a slightly vague text message from a partner might trigger an immediate, catastrophic fear of abandonment, resulting in impulsive texting or calling them twenty times in a row.
Another classic example is the sudden emotional shutdown after a stressful day at work.
Instead of feeling appropriately tired, the individual’s nervous system becomes so overloaded by the emotional effort of masking their distress that they come home and experience sudden anger or uncontrollable crying over a minor inconvenience, like a misplaced set of keys.
We also see Bipolar vs. Emotional Dysregulation Differences present as severe financial or social impulsivity to escape negative feelings.
A person might feel a sudden spike of anxiety and immediately cope by spending a thousand dollars online or abruptly quitting a job to relieve the immediate emotional pressure.
Conditions Often Confused With Emotional Dysregulation
When exploring what can be mistaken for emotional dysregulation, we must carefully differentiate between mood disorders, complex trauma, and neurodevelopmental nuances like avoidant personality disorder vs autism.
A frequent source of diagnostic confusion is emotional dysregulation in ADHD, which frequently overlaps with the rapid emotional shifts seen in ADHD and BPD.
In ADHD, individuals often suffer from Rejection Sensitive Dysphoria (RSD), meaning they experience intense emotional pain perceived as physical pain when they feel criticized, but this is linked to executive dysfunction, not cyclical manic episodes.
Another concept I frequently explain in my practice is alexithymia. This is not a disorder itself but a personality trait characterized by the severe inability to identify, understand, and describe one’s own emotions.
When a person has alexithymia, they may experience profound physiological arousal—like a racing heart or sweating—but cannot attach an emotional label to it, leading to explosive frustration that mimics dysregulation.
Finally, trauma responses, such as Complex PTSD, are frequently mislabeled. Chronic childhood trauma alters the brain’s neuroplasticity, leaving the nervous system stuck in a state of hypervigilance that is highly reactive to environmental triggers, completely independent of the circadian rhythms that govern bipolar disorder.
Treatment & Emotional Regulation Strategies

Finding the right treatment for Bipolar vs. Emotional Dysregulation requires a highly individualized, patient-centered approach.
I always caution my patients that there are no instant cures, but there are highly effective, evidence-based emotional regulation strategies that can dramatically improve their quality of life.
For Bipolar vs. Emotional Dysregulation Differences, psychiatric medication is almost always the necessary foundation. Mood stabilizers and atypical antipsychotics calm the hyperactive limbic system, lowering the baseline level of neurochemical distress so that psychological therapies can actually take root.
Once the brain is chemically stabilized, we turn to therapies like Dialectical Behavior Therapy (DBT). DBT is the gold standard for teaching patients how to tolerate severe distress without acting impulsively, using grounding techniques to force the prefrontal cortex back online.
Cognitive Behavioral Therapy (CBT) is also vital for emotional awareness training, helping patients identify the distorted thoughts that fuel their rapid emotional escalation.
I consistently have patients utilize trigger tracking—logging their sleep, stress levels, and emotional spikes daily—to predict and prevent episodes before they spiral out of control.
ESA Documentation vs Emotional Support Context
In the context of seeking emotional regulation support, patients occasionally ask about incorporating animals into their treatment plan. It is helpful to briefly clarify the landscape of emotional support animals (ESAs) as an adjunctive coping tool.
Many individuals search for information on printable ESA letters vs. regular pet documentation: what’s the difference?
Legally and clinically, a valid ESA letter must be written by a licensed mental health professional who is actively treating you, explicitly stating that the animal provides necessary therapeutic support for your diagnosed condition.
This documentation is entirely different from a standard veterinary pet record, and it is also distinct from service animal certifications.
While an ESA can provide profound comfort and routine-building benefits during depressive crashes, obtaining proper, legitimate documentation through your actual care provider is essential to avoid online scams.
Frequently Asked Questions
Differentiating Rapid Mood Swings?
Mood instability in emotional dysregulation is highly reactive to the environment and can shift within minutes. Bipolar mood swings, even in rapid-cycling forms, are neurological episodes that generally last for days or weeks and occur regardless of external stressors.
The Role of Self-Assessments?
Taking a self-test is a powerful first step in organizing your thoughts and recognizing destructive patterns. However, it should strictly be used to spark a conversation with a licensed psychiatrist or psychologist, never to self-diagnose.
Managing Sudden Emotional Impulsivity?
The most effective strategy for sudden impulsivity is enforcing a “clinical pause.” Patients are taught to physically step away from the triggering environment and use cold water therapy or paced breathing to reset their nervous system before responding.
Impact of Sleep on Emotion?
Sleep deprivation directly attacks the brain’s executive function. Without adequate rest, your brain cannot filter out unnecessary emotional data, making you highly vulnerable to intense dysregulation and triggering bipolar mood episodes.
Effectiveness of Therapeutic Intervention?
Therapy does not erase bipolar vs. Emotional Dysregulation Differences, but it radically alters your relationship with them. By actively practicing distress tolerance skills, patients can structurally alter their brain’s neuroplasticity, making future emotional responses less severe and more manageable.
Conclusion
Understanding the deep nuances of your own mind is the bravest undertaking you can commit to. In my practice, the moment a patient realizes that their intense, frightening emotional reactions are the result of neurobiology—and not a personal moral failing—is the moment true healing begins.
Whether you are navigating the Bipolar vs. Emotional Dysregulation Differences or the rapid-fire triggers of emotional dysregulation, you are not broken. Your nervous system is simply communicating distress in the only way it currently knows how.
If you are seeing your own reflection in these signs of bipolar disorder, when should you take a self-test? Let that self-reflection be your catalyst. Reach out to a mental health professional, prioritize your circadian rhythms, and begin the deeply rewarding work of reclaiming your emotional peace.
Authoritative References
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.