Criteria for PTSD: A Complete Guide for Veterans

Medically reviewed by Laura Athey Updated Date: May 4, 2026
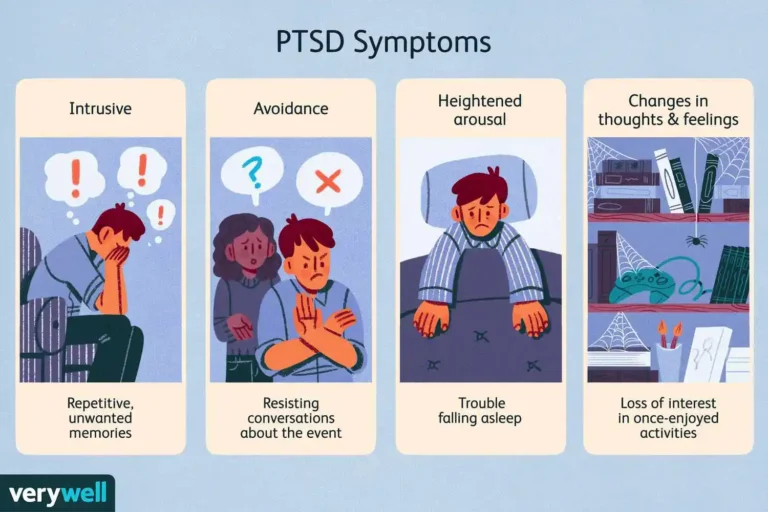
For many veterans, the transition from active duty to civilian life isn’t just a change in career—it’s a move from a world of high-stakes alertness to an environment that feels dangerously quiet.
Posttraumatic Stress Disorder (PTSD) is often the invisible passenger on that journey. However, navigating the clinical criteria for PTSD while simultaneously fighting for a VA disability rating can feel like a second deployment.
In my years of clinical practice, I have interviewed hundreds of veterans who feel “stuck” between a medical system that categorizes their pain and a VA system that quantifies it.
I recently worked with a former Marine, “Jack,” who had spent a decade suppressing memories of a combat engagement in Fallujah.
He came to me because he was losing his job. “I can’t focus,” he said. “Every time a car backfires or a door slams, I’m back in the turret. But the VA says I’m only 30% disabled because I still show up to work most days.”
Jack’s story illustrates the vital need for a deep understanding of the DSM-5-TR criteria for PTSD and how those clinical benchmarks translate into VA disability rating criteria. This article serves as a comprehensive resource to bridge that gap.
What Are the DSM-5-TR Diagnostic Criteria for PTSD?
The DSM-5-TR (Text Revision) is the gold standard for mental health professionals. To receive a formal diagnosis, a veteran must meet a specific number of symptoms within several “clusters.”
The 8 Key Clusters: How Many Criteria for PTSD?
Many people ask, “How many criteria for PTSD?” Technically, there are eight major criteria (A through H), but within those, there are specific symptom counts required.
Criterion A: Trauma Exposure (1 Required) You must have been exposed to death, threatened death, serious injury, or sexual violence in one of the following ways:
- Direct Exposure: You were there.
- Witnessing: You saw it happen to someone else.
- Indirect Exposure: Learning that a close friend or family member was exposed to trauma.
- Repeated Exposure: Common for medics, first responders, or drone operators (Secondary Traumatic Stress).
Criterion B: Intrusion Symptoms (1 Required) The trauma is persistently re-experienced through:
- Recurrent, involuntary, and intrusive memories.
- Distressing dreams (nightmares).
- Dissociative reactions (flashbacks) where you feel the event is recurring.
- Intense or prolonged psychological distress at “triggers.”
Criterion C: Avoidance (1 Required) Persistent avoidance of stimuli associated with the trauma:
- Avoiding thoughts or feelings related to the event.
- Avoiding external reminders (people, places, conversations, or military gear).
Criterion D: Negative Alterations in Cognition and Mood (2 Required) This cluster covers how your world-view changed:
- Inability to remember key aspects of the trauma (dissociative amnesia).
- Persistent, exaggerated negative beliefs about oneself or the world (“I am bad,” “The world is completely dangerous”).
- Distorted blame of self or others.
- Persistent negative emotional state (fear, anger, guilt, shame).
- Feeling alienated or detached from others.
Criterion E: Alterations in Arousal and Reactivity (2 Required) Your nervous system is “always on”:
- Irritable behavior and angry outbursts.
- Hypervigilance (scanning the room, sitting with your back to the wall).
- Exaggerated startle response.
- Problems with concentration.
- Sleep disturbance.
Criteria F, G, and H: The Fundamentals
- Duration: Symptoms must last more than one month.
- Impairment: The symptoms cause significant distress or impairment in social, occupational, or other functional areas.
- Exclusion: The disturbance is not due to substances or other medical conditions.
PTSD DSM-5 Codes & Documentation for VA Claims
When filing a claim, the clinical language matters. What is the dsm-5 criteria code for ptsd? The question is simple but vital for your paperwork: it is the ICD-10-CM code F43.10.
Importance of the PTSD Criteria PDF & Checklist
Clinicians use a DSM-5 PTSD criteria checklist to ensure they haven’t missed a cluster. For veterans, having a PTSD DSM-5 criteria PDF summary can help you articulate your symptoms to a C&P (Compensation and Pension) examiner.
In Jack’s case, we found that he was under-reporting his “Criterion D” symptoms (shame and blame) because of the “warrior culture” of silence, which significantly impacted his initial rating.
VA Disability Rating Criteria for PTSD
The VA does not give a rating based on the presence of PTSD alone. They give it based on how much the PTSD interferes with your ability to work and live. This is the core of the VA rating criteria for PTSD.
Understanding the Rating Percentages
- 0%: A mental condition has been formally diagnosed, but symptoms are not severe enough to interfere with social or occupational functioning.
- 10%: Occupational and social impairment due to mild or transient symptoms, or symptoms controlled by continuous medication.
- 30%: Occupational and social impairment with occasional decrease in work efficiency and intermittent periods of inability to perform occupational tasks.
- 50%: Occupational and social impairment with reduced reliability and productivity. Common signs include panic attacks more than once a week, difficulty understanding complex instructions, or impaired judgment.
- 70%: Occupational and social impairment in most areas (work, school, family, judgment, thinking, or mood). Symptoms include suicidal ideation, near-continuous panic/depression, and inability to maintain relationships.
- 100%: Total occupational and social impairment. This may involve gross impairment in communication, persistent delusions/hallucinations, or being a danger to self/others.
What Is the Average PTSD Claim Rating From the VA? While it varies, the most common rating for a successful PTSD claim is 70%, followed by 50%. A 100% rating is difficult to achieve without significant evidence of total inability to function in a work environment.
Who Can Diagnose PTSD for VA Disability?
To satisfy the criteria for diagnosing PTSD for a VA claim, the diagnosis must come from a qualified professional.
- Psychiatrists (MD/DO): Medical doctors who can manage medication.
- Clinical Psychologists (PhD/PsyD): Specialists in diagnostic testing.
- VA C&P Examiners: Contracted or VA-employed providers specifically trained to evaluate claims.
Important Note: While a Licensed Clinical Social Worker (LCSW) or Licensed Professional Counselor (LPC) can provide excellent treatment, the VA often requires a signature from a PhD-level psychologist or a psychiatrist for the initial “Nexus” (link) to service.
PTSD in Special Veteran Populations
The impact of military trauma often ripples through the entire family unit, leading to unique diagnostic challenges.
PTSD in Children of Veterans
Intergenerational trauma is a documented phenomenon. When looking at the criteria for ptsd in children, specifically DSM-5 PTSD criteria under 6, the symptoms manifest differently.
Instead of talking about their feelings, children may engage in “play reenactment,” where they repeatedly play out scenes of trauma. They may show “frightening dreams” without recognizable content or exhibit extreme social withdrawal.
Chronic & Complex PTSD
While the criteria for ptsd chronic historically referred to symptoms lasting over six months, the DSM-5-TR focuses on “delayed expression.” Some veterans do not manifest full criteria until years after they separate from service.
Furthermore, Complex PTSD (CPTSD) is a term frequently used by trauma specialists. While Complex PTSD DSM-5 criteria are not formally separated from standard PTSD in the current manual, the ICD-11 (used by the WHO) does recognize it.
CPTSD involves the standard PTSD clusters plus “disturbances in self-organization,” such as chronic feelings of worthlessness and extreme difficulty maintaining emotional stability.
What Are the Symptoms of PTSD?
Beyond the clinical manual, understanding the “hallmarks” of the disorder helps veterans recognize their own patterns.
What are the 4 hallmarks of PTSD?
These align with the DSM clusters:
- Intrusion: Memories that won’t go away.
- Avoidance: Running from reminders.
- Negative Changes: Loss of hope or joy.
- Hyperarousal: Living on a “hair trigger.”
What are the 5 F’s of PTSD?
This is an educational framework for understanding the “survival brain.”
- Fight: Irritability and aggression.
- Flight: Social withdrawal or work-avoidance.
- Freeze: Feeling “stuck,” numb, or unable to make a decision.
- Fawn: Trying to please everyone to avoid conflict (common in MST survivors).
- Fragment (or Flop): Dissociating or “spacing out” when the stress is too high.
What If You Don’t Meet Full PTSD Criteria?
If you have symptoms but don’t hit every “check” on the dsm criteria for ptsd unspecified list, you may be diagnosed with Other Specified Trauma- and Stressor-Related Disorder.
This is not a “lesser” diagnosis. For VA purposes, an “unspecified” diagnosis can still result in a disability rating if it causes occupational and social impairment. Don’t stop seeking treatment just because you don’t meet every single one of the 4 diagnostic criteria for ptsd.
How Is PTSD Treated?
Once you have a diagnosis, the goal shifts to recovery. How is PTSD treated? The VA and private clinics prioritize “evidence-based treatments” (EBTs).
- Cognitive Processing Therapy (CPT): Helps you challenge and change the “stuck points”—the negative beliefs you’ve held since the trauma (e.g., “It was my fault”).
- EMDR (Eye Movement Desensitization and Reprocessing): Uses bilateral stimulation (eye movements or taps) to help the brain re-process traumatic memories so they no longer carry a “charge.”
- Prolonged Exposure (PE): Gradually helps you re-engage with the things you’ve been avoiding because of your trauma.
- Medication: SSRIs (like Zoloft or Paxil) are commonly used. Prazosin is frequently prescribed to veterans specifically for trauma-related nightmares.
Do You Need an Accredited VA Claims Lawyer?
Filing a claim for PTSD can be overwhelming. Do You Need an Accredited VA Claims Lawyer for PTSD Claims? * If it’s your first time: Most veterans can work with a Veteran Service Officer (VSO) for free.
- If you’ve been denied, an accredited lawyer or agent may be helpful for navigating the “Board of Veterans’ Appeals.” They understand how to argue “Total Occupational and Social Impairment” when the C&P examiner missed the mark.
When PTSD and Mood Cycling Overlap
In the veteran community, the diagnostic boundary between PTSD and Bipolar Disorder is frequently blurred.
In my clinical experience, the “hyperarousal” seen in the DSM-5-TR criteria for PTSD can mirror the agitation of a hypomanic episode, while the “negative alterations in mood” can be indistinguishable from bipolar depression.
This is particularly relevant for veterans who may be misdiagnosed when their trauma-induced “flight” response is mistaken for the racing thoughts of mania.
However, a key differentiator lies in the trigger. PTSD symptoms are typically “reactive” to external reminders or internal triggers, whereas bipolar cycles often follow a more autonomous biological rhythm.
For those navigating the VA rating criteria for PTSD, it is essential to have a provider who can disentangle these conditions. An accurate diagnosis ensures you aren’t just treating the “mood” with medication, but also addressing the underlying “nervous system injury” through trauma-focused therapy.
Frequently Asked Questions
What is the DSM-5 criteria for PTSD?
It is a set of eight requirements (A–H) involving exposure to a traumatic event and subsequent symptoms of intrusion, avoidance, negative mood changes, and hyperarousal lasting more than a month.
What are the DSM-5-TR criteria for PTSD?
The “TR” stands for Text Revision. The core criteria remain the same as the DSM-5, but it provides updated language to clarify the “Negative Alterations in Cognition and Mood” cluster and better describes trauma in marginalized populations.
How many criteria are required for PTSD?
To be diagnosed, you must have: 1 Criterion A (trauma), 1 Criterion B (intrusion), 1 Criterion C (avoidance), 2 Criterion D (mood), and 2 Criterion E (arousal) symptoms, plus meeting the duration and impairment requirements (F, G, H).
Who can diagnose PTSD?
For official medical records and VA claims, only a licensed psychiatrist (MD/DO) or a clinical psychologist (PhD/PsyD) should provide the formal diagnosis.
What is the PTSD DSM-5 code?
The clinical code used for insurance and medical billing is ICD-10-CM F43.10.
Conclusion
Your military service ended, but for many, the “internal battle” continues. Understanding the diagnostic criteria for ptsd is not about accepting a label; it’s about gaining a map.
Whether you are filing a VA claim for PTSD or simply trying to explain to your family why you can’t go to the crowded mall, knowledge is your strongest asset.
At our clinic, we focus on providing veterans with the diagnostic clarity they need to access both the benefits they earned and the treatment they deserve. You don’t have to carry the rucksack alone anymore.
References
- American Psychiatric Association: DSM-5-TR Fact Sheet on PTSD
- U.S. Dept of Veterans Affairs (VA): PTSD Rating Schedule (38 CFR § 4.130)
- National Center for PTSD: Research and Treatment Resources
- The Lancet Psychiatry: Advances in the Treatment of Military-Related PTSD
Subscribe to Our Newsletter
Get mental health tips, updates, and resources delivered to your inbox.










